Dr. Jessica Dorsey is board-certified both as a dermatologist and Micrographic Dermatologic Surgeon. She is also a fellowship-trained Mohs surgeon.
Dr. Dorsey graduated with Honors with her degree in Biology, focusing on health sciences from East Carolina University. After working three years in clinical research at a contract research organization, Dr. Dorsey attended medical school and completed her internal medicine internship at Texas Tech University & Texas A&M University Health Sciences College of Medicine. Her dermatology residency was completed in Temple, Texas at Scott & White Hospital, where she served as chief resident. Dr. Dorsey completed her training with a Mohs micrographic surgery & reconstruction fellowship under the direction of Dr. Glenn Goldstein in Kansas City.
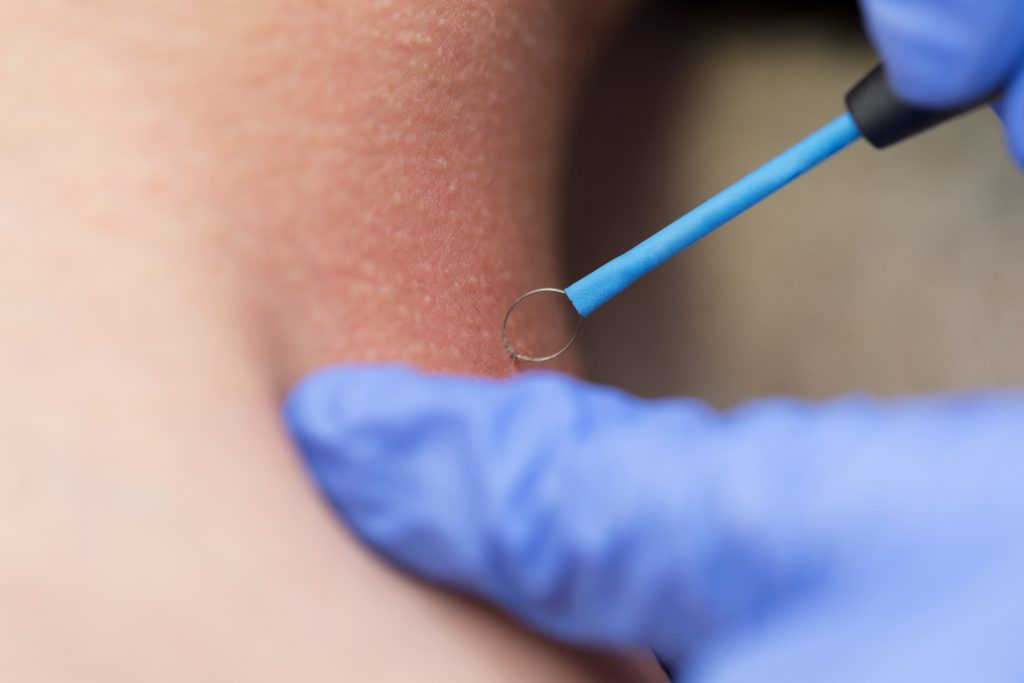
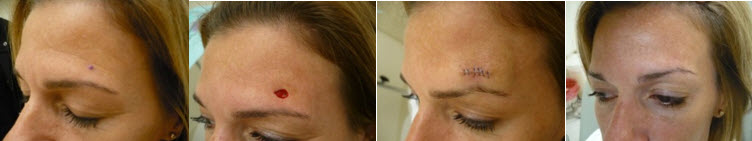
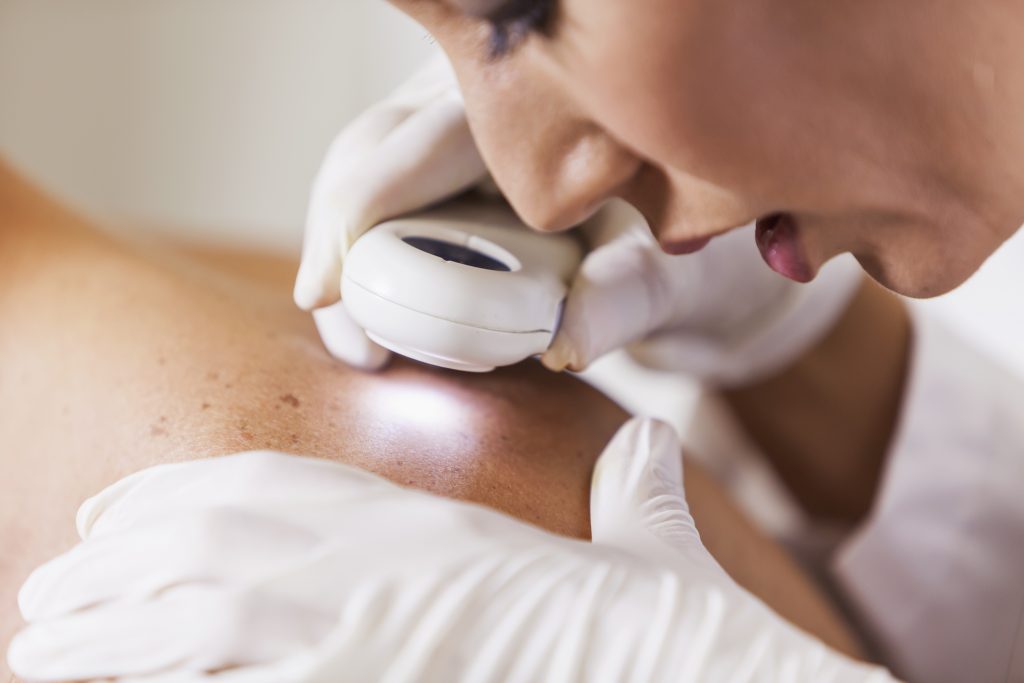
Dr. Dorsey’s clinical interest and specialty is skin cancer, Mohs surgery and facial reconstruction, dermatologic surgery and nail surgery. Not only does she perform Mohs surgery for basal cell carcinoma, squamous cell carcinoma, and other complex skin cancers, but she also offers Mohs surgery for melanoma in situ. This requires the use of immunohistochemistry stains which highlight melanoma cells in the skin, allowing the ability for a lower risk of recurrence, higher cure rate, and increased capability for tissue-sparing in complex sites. In addition, it often results in immediate reconstruction after obtaining clear margins without the need for multiple visits in order to test the tissue. Dr. Dorsey has performed over 10,000 surgical cases.
Dr. Dorsey is a diplomate of the American Board of Dermatology, a Fellow of the American Academy of Dermatology, and a Fellow of the American College of Mohs Surgery. In her spare time, Dr. Dorsey enjoys cooking, travel, and spending time with her husband and daughter, cats, dogs, goats and llamas.
Dr. Jessica Dorsey treats patients at our Cedar Park office.
Badges & Awards
Specialties and Affiliations
- American Board of Dermatology
- American College of Mohs Surgery
Featured Blogs
- Bruising and Swelling After Mohs Surgery: What’s Normal and How to Treat It
- 30 U.S. Dermatology Partners Physicians Recognized as 2025 Super Doctors® in Texas
- 42 U.S. Dermatology Partners Physicians Recognized by 2024 Super Doctors® Awards
- Fight Skin Cancer: Learn About BCC & Prevention
- Super Doctors 2023 Recognizes 43 U.S. Dermatology Partners Physicians in Peer-Nominated Award
- Thirty-One U.S. Dermatology Partners Dermatologists Across Texas Received Super Doctor & Rising Star Awards
- What Types of Skin Cancers are Deadly?
- Texas Monthly Super Doctors 2020 Recognizes 35 U.S. Dermatology Partners Physicians in Peer-Nominated Award
- U.S. Dermatology Partners Cedar Park is Pleased to Announce its Relocation
- Dermatologists' Top Skin Care Tips for Moms
- Texas Monthly Recognizes 26 U.S. Dermatology Partners Physicians