Mole Treatments from U.S. Dermatology Partners
What Are Moles?
Atypical moles, also known as dysplastic nevi, are unusual-looking benign (noncancerous) moles.
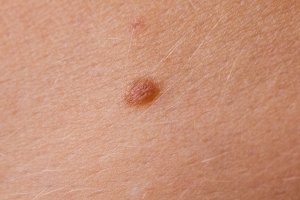
A dysplastic mole is one that, when viewed on a cellular level, has features unlike those of a healthy, benign mole. A benign mole will have a regular pattern of coloration and pigment, even borders, symmetry, and a tan or pink color. Dysplastic moles can be asymmetric, have indistinct borders, or contain multiple colors or very dark pigment.
Dysplastic moles are often spotted as the “ugly duckling” on a patient’s skin. Any departure from the typical mole a person’s skin makes may be dysplastic. They can appear anywhere on the body, but in most cases are found on the back, chest, buttocks, breasts, or scalp.
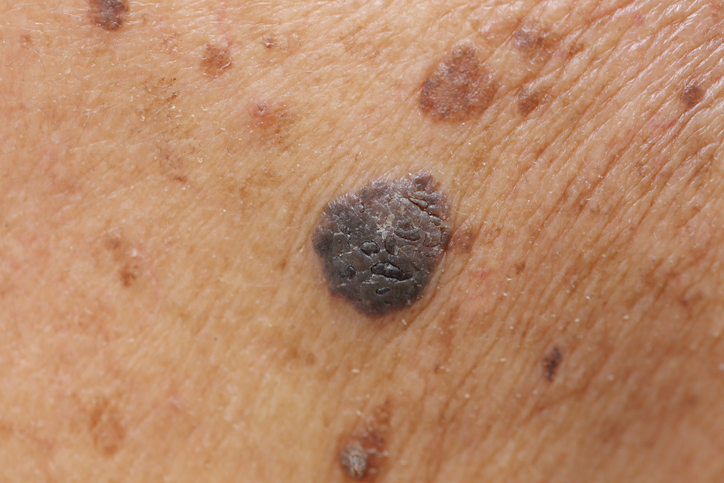
People with atypical moles are at a higher risk of developing melanoma.
Find This Service Near You
Who Is at Risk for Moles?
Heredity plays a major role in dysplastic nevi. The condition runs in families, especially in Caucasians. Individuals with 10 or more dysplastic nevi moles have 12 times the risk of developing melanoma compared to the general population – and the risk increases further if family members also have atypical moles.
Even without a family history of melanoma, people with atypical moles run a greater risk of developing melanoma than the general population.
3 Types of Atypical Moles
Everyone has moles and they can appear in both sun-exposed and sun-protected areas. Though dysplastic nevi often resemble melanoma, they are noncancerous.
Most moles can be classified in one of three ways:
Flat Moles
Flat moles, which refer to a dark or irregular spot in the skin.
Raised Moles

Skin Tags
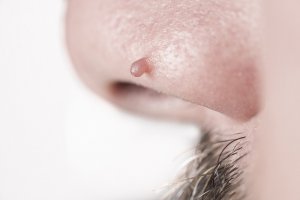
There are several ways to determine if a mole should be biopsied, monitored, or removed. If a mole changes or becomes symptomatic. it should be evaluated by a dermatologist. In addition to regular monitoring by your doctor, you should also monitor your moles regularly at home.
Are Dysplastic or Atypical Moles Cancerous?
Dysplastic moles are not yet cancerous nor are they considered “pre-cancerous,” only potentially so.
Dysplasia comes in varying degrees, from mild to moderate to severe. The risk of melanoma development generally correlates with the severity of abnormality noted. Mildly atypical moles can be monitored for regrowth and future changes. Moderately and severely atypical moles will often be completely removed following a biopsy, as these more extreme changes may indicate a high potential for development into melanoma. For this reason, it is best to remove the mole completely to avoid any further evolution.
This does not mean the mole was necessarily going to become a melanoma, but, due to the danger of this type of cancer, it is best to use precaution.
Monitoring Your Moles
If you have had multiple dysplastic moles, you are at higher risk for having more atypical moles (and possibly melanoma) in the future. Dysplastic moles are more likely to develop into melanoma than are benign moles, which rarely evolve into anything dangerous.
This does NOT mean you WILL have melanoma if you have dysplastic moles; most remain stable over time. It does, however, mean your skin needs to be watched more closely and that you need to take certain precautions:
- See your dermatologist for skin exams every 6-12 months, or more depending on the provider’s recommendation.
- Be diligent with wearing daily sun protection of SPF 30+ on exposed areas to avoid atypical changes in your moles.
- Make a habit to screen yourself monthly. Some people like to take photos for a reference point or have a spouse or friend look at areas that are hard for you to see.
When in doubt, always have a professional dermatologist evaluate any and all areas of concern. Skin cancer is very treatable when caught early, so it is always best to err on the side of caution when you have a concern. Click here to request an appointment with a Board-Certified Dermatologist.
Mole Treatments
If your doctor identifies your moles as atypical, or if new moles appear after age 40, you may need a biopsy of one or more of the moles. If the mole is benign, you will simply need to continue with self-examination and prevention.
If your doctor recommends that a mole be removed, the procedure is typically very quick with little or no downtime post-procedure. Moles may be treated using cryotherapy.
Mole Prevention
Your doctor should conduct a baseline examination and determine which moles, if any, are abnormal enough to be biopsied or removed.
The doctors at U.S. Dermatology Partners can provide more information about the risk of dysplastic nevi and recommend a treatment plan for you.
*Results may vary by individual