Treatments for Hyperhidrosis & Excessive Sweating from U.S. Dermatology Partners
What is Hyperhidrosis?
Hyperhidrosis, often referred to as excessive sweating, occurs when people experience disproportionate and/or unnecessary sweat production. While sweating is a natural function of the body’s systems to keep itself cool and maintain the best temperature, sweating too much or sweating that is not necessary to cool the body can create many difficulties that impact your overall health and wellbeing. Generalized hyperhidrosis may affect the whole body. Others have localized cases of excessive sweating that impact only certain areas. Specifically, there are three main types of localized hyperhidrosis: axillary (impacting the underarms), palmar (impacting the palms), and plantar (impacting the feet). If you experience general or localized excessive sweating at least once per week, you should talk to a dermatologist about a treatment plan.

There are three main types of localized hyperhidrosis: axillary (impacting the underarms), palmar (impacting the palms), and plantar (impacting the feet).
Find This Service Near You
Who is at Risk for Hyperhidrosis?
Anyone of any age may be at risk for hyperhidrosis, but it is most often diagnosed in the adolescent years. As bodies develop and hormone levels increase, this excessive sweating condition typically becomes clear. The underlying cause of excessive sweating is overactive eccrine glands that are responsible for sweat production and regulating body temperature. While the overactive glands clearly lead to hyperhidrosis, no specific cause for this excessive sweat production is evident in most cases. For this reason, most diagnosed cases of hyperhidrosis are designated as idiopathic, which means the cause is unknown.
While the specific factor that leads to excessive sweat production is typically unclear, genetics is almost certainly a factor. If one or more of your family members suffers from this condition, you are much more likely to develop hyperhidrosis. In rare cases, certain medications and health conditions can contribute to excessive sweating. During an appointment with the U.S. Dermatology Partners team, we will review your family history, personal health history, current medications, and recent injuries to ensure we offer the most accurate diagnosis and effective treatment plan.
Hyperhidrosis Symptoms
In order to determine whether you are suffering from hyperhidrosis, you will need to receive an official diagnosis from a dermatologist.
We recommend scheduling an appointment if you notice any of the following symptoms:
- Clammy or wet palms of the hands
- Clammy or wet soles of the feet
- Frequent sweating
- Noticeable sweating that soaks through clothing
- Chronic irritating and painful skin problems, such as fungal or bacterial infections
In addition to these physical symptoms, people with hyperhidrosis might also experience the following adverse effects:
- Worrying about or hiding stained clothing
- Reluctance to make physical contact
- Self-consciousness about the condition
- Withdrawing socially potentially leading to depression
- Limiting employment to positions where physical contact or regular interaction is not a requirement
- Spending a large amount of time dealing with sweat by changing clothes, showering/bathing frequently, placing napkins or pads under the arms, washing, and wearing bulky or dark clothes
- Worrying more than other people about body odor
Hyperhidrosis Treatment
During a diagnosis appointment, a dermatologist will ask you a number of questions to help determine what the underlying causes of your condition may be. If it’s discovered that illness, injury, or medication has caused excessive sweating, you’ll be advised to take steps to treat these conditions and reduce the impact of hyperhidrosis on your life. If your condition is considered genetic and/or idiopathic, there are still many treatments available to relieve side effects and improve your experience. We will usually recommend some combination of the following treatment options.
Over the Counter & Prescription Strength Antiperspirants
The first place to start is usually with over the counter antiperspirants that can be used to dry sweat glands and prevent sweat production. If over the counter antiperspirants are ineffective, prescription-strength options may be a good choice. With daily use, many people see dramatic improvement of symptoms, namely reduced sweat production.
Topical & Oral Anticholinergics
If antiperspirant doesn’t deliver the desired results, we may recommend an anticholinergic. These are typically provided as topical ointments or oral medications. They reduce sweat production by blocking overactive neurotransmitters that lead to excessive sweating. While they have shown to be successful in treating hyperhidrosis, the efficacy of these medications has not been studied specifically regarding treatment for excessive sweating. However, the FDA has approved usage based on the results of studies that proved successful treatment of similar conditions.
Iontophoresis
For those suffering from certain forms of localized excessive sweating, namely plantar and palmar hyperhidrosis, iontophoresis may be recommended. This treatment process requires the impacted extremities (hands or feet) to be placed in water. A low-voltage electrical current is then passed through the water. This procedure freezes the sweat glands, and in many cases, just one treatment is shown to dramatically reduce sweat production for hours, days, and even weeks. In most cases, six to ten treatments will be recommended, and after completing the series of iontophoresis treatments, many people find total relief from the effects of excessive sweating.
Neurotoxin Injections
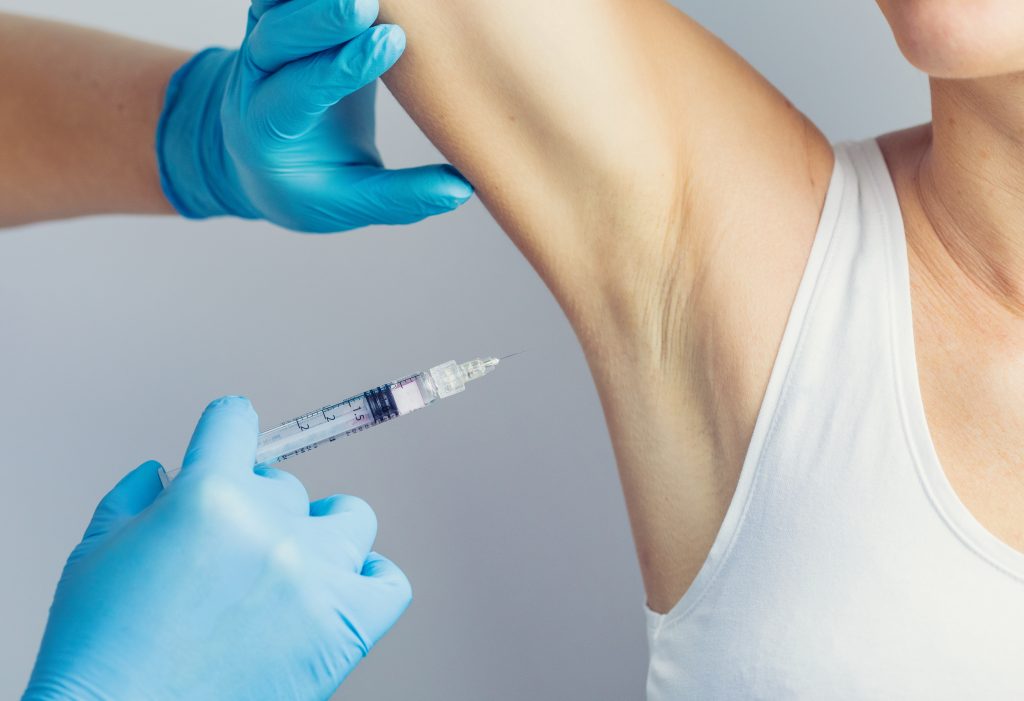
The treatment itself uses a controlled level of neurotoxin that is injected into the area(s) affected by excessive sweating and hyperhidrosis.
While neurotoxins such as Botox, Dysport, Jeuveau, and Xeomin are most commonly associated with the reduction of fine lines and wrinkles, they can also be used to reduce muscle movements that lead to strain and discomfort, and today, we can utilize these injection treatments for a variety of conditions. The treatment itself uses a controlled level of neurotoxin that is injected into the area(s) affected by excessive sweating. This reduces nerve impulses that stimulate sweat production. Over time, the injections limit the nerve stimulus, and they can reduce sweating for months at a time. Each person’s condition is unique, so we will create a personalized neurotoxin plan to improve your hyperhidrosis.
Surgery
If no other treatments have been effective and your condition is negatively impacting your daily life, we may recommend surgical intervention. Typically, the recommended procedure is called a thoracic sympathectomy. This procedure interrupts a section of the sympathetic nerve system that is in control of sweat production. These procedures are particularly effective for those who are diagnosed with localized hyperhidrosis as it can be difficult to stop sweating in all parts of the body without adversely affecting the body’s entire temperature regulation system.
Hyperhidrosis Prevention
In most cases, hyperhidrosis cannot be prevented, but by developing an effective treatment plan, you can prevent many of the most serious symptoms.
Some tips to limit excessive sweating include:
- Avoid high temperatures or prolonged activity that can increase sweating
- Apply antiperspirants to affected areas to prevent sweating
- Take prescribed medications and follow other dermatologist recommendations
- Take steps to reduce stress and anxiety
If you are experiencing hyperhidrosis and want to work with one of our skilled dermatologists, get started by completing our online request form. One of our knowledgeable team members will be in touch to schedule your visit with us. With our extensive network of providers throughout Arizona, Colorado, Kansas, Maryland, Missouri, Oklahoma, Texas, and Virginia, there’s a U.S. Dermatology Partners practice near where you live or work.
*Results may vary by individual

