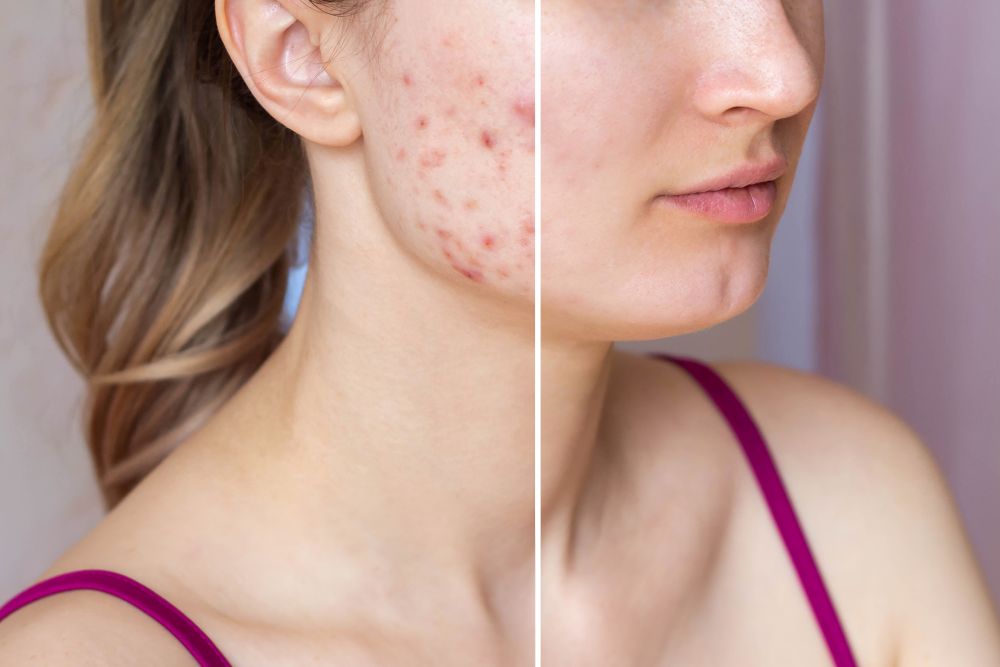
Acne vulgaris, often referred to simply as acne, is the most common skin condition treated by dermatologists, impacting as many as 50 million people in the U.S. annually. According to Dr. Emily Clarke of U.S. Dermatology Partners Austin – Mueller, “Many people who seek dermatologic care are dealing with some form of acne. While many people who suffer from acne are teens, I also see adults who are managing acne breakouts. Some people struggling with acne may feel hopeless about achieving clear skin, especially if prior treatments haven’t worked. Fortunately, there are many treatment options available that can target different types of acne. As a dermatologist, I partner with my patients to achieve and maintain clear skin. That all starts with developing a personalized treatment plan based on the type of acne and the goals of my patient.” In this blog, Dr. Clarke discusses three common types of acne, their causes, and the best treatment approach for each.
Three Common Types of Acne
There are different types and severities of acne, which will be reviewed in this blog. According to Dr. Clarke, “Your dermatologist may categorize acne based on the type of blemishes they see on your skin, thereby ensuring they can recommend the best treatment options.” Below, Dr. Clarke describes three common types of acne encountered by dermatologists.
Comedonal Acne
Comedonal acne is one of the most common forms of acne seen by dermatologists. It involves the development of open comedones (blackheads) and closed comedones (whiteheads). This form of acne is not usually painful or inflamed. It often develops in the “T-Zone” of the face, including the forehead, nose, and chin due to clogged pores. Pores may clog with naturally produced oils (sebum), dead skin cells, and other debris. If the clogged pore remains open, the oxygen exposure causes it to appear black, creating an open comedone or “blackhead.” If the clogged pore is covered by skin, it forms a closed comedone or “whitehead.” A comedonal acne breakout may be triggered by excessive sebum production, skincare or hair products, and changes in hormones. To prevent comedonal acne, it is important to ensure that all skin care products used are “oil-free” and “non-comedogenic,” which means they do not cause acne.
Some treatments for comedonal acne include:
- Gentle cleansers – maintaining a consistent cleansing routine is essential. Wash skin twice a day with a mild cleanser to clear pores without drying skin.
- Salicylic acid – using a gentle salicylic acid wash can break down oil and debris in pores, preventing the formation of new pimples.
- Benzoyl peroxide – reduces acne-causing bacteria and helps prevent inflammation.
- Topical retinoids – these topical products are considered the gold standard for comedonal acne management. They increase skin cell turnover and decrease sebum production, preventing clogged pores and smoothing texture.
Inflammatory Acne
Inflammatory acne breakouts are made up of red bumps and pimples that may be sore or swollen. The red bumps that do not contain pus are known as “papules,” while the larger pimples with a pus-filled center are known as “pustules.” Inflammatory acne develops when clogged pores trigger an immune response to bacteria and trapped sebum. This increased immune response around the pore filled with trapped sebum and bacteria leads to symptoms of warmth, redness, swelling, tenderness, and pain. Sometimes women can get a type of inflammatory acne called “hormonal acne” that presents along the jawline and chin, often flaring with menstrual cycles.
Some treatments for inflammatory acne include:
- Benzoyl peroxide – reduces acne-causing bacteria, helps prevent inflammation, and decreases the risk of developing antibiotic resistance when combined with antibiotics.
- Topical antibiotics – may be used as a maintenance treatment to prevent pimples or during an inflammatory acne breakout to reduce bacteria and inflammation.
- Topical retinoids – increase skin cell turnover and decrease sebum production.
- Oral antibiotics – improve more severe flares of pimples by reducing bacteria and inflammation faster and more effectively than topical antibiotics.
- Hormonal therapies – hormonal therapies may be recommended for women with inflammatory acne on the chin or jawline that flares with menstrual cycles.
Nodulocystic Acne
The most severe form of acne is nodulocystic acne. It’s made up of painful, deep acne bumps called cysts and nodules. Nodulocystic acne occurs when inflammatory acne extends more deeply into the skin. These nodules and cysts are often swollen, red, and painful to the touch. Sometimes they may drain pus or bleed. Nodulocystic acne breakouts may be longer in duration than other forms of acne, lasting for weeks or even months. Without treatment from a dermatologist, nodulocystic acne may result in skin color changes and scarring. It’s essential to seek treatment as soon as possible for nodulocystic acne as early treatment can reduce the risk of permanent scarring.
Some treatments for nodulocystic acne include:
- Oral antibiotics – improve more severe flares of nodulocystic acne by reducing bacteria and inflammation faster and more effectively than topical products.
- Isotretinoin – one of the most powerful acne medications available, often recommended for nodulocystic acne with the goal of reducing active acne and preventing scarring. Isotretinoin is typically reserved for moderate-severe, scarring, or treatment-resistant acne.
Best Dermatologist-Approved Treatments
Acne treatment may include your at-home acne skincare routine, medications prescribed by your dermatologist, as well as in-office dermatologic procedures. The right treatment options will be determined in partnership with your dermatologist based on your skin health and the type of acne. Dr. Clarke outlines the most frequently recommended dermatology treatments below.
At-Home Products
Proper acne treatment starts with a consistent at-home care routine that includes the best products for acne. It’s important to be patient and persistent. At-home treatment often takes between six and twelve weeks to achieve the desired results. Dermatologist-recommended at-home acne skincare includes:
- Gentle cleansers – washing the skin twice a day with a mild cleanser to clear pores without causing dryness. Avoid harsh cleansers or abrasive exfoliants that irritate the skin.
- An over-the-counter medicated face wash – salicylic acid or benzoyl peroxide face washes can reduce clogged pores and acne-causing bacteria.
- An “oil-free,” “non-comedogenic” moisturizer – this is a way to promote a healthy skin barrier and prevent dryness from acne treatments while avoiding clogged pores that can cause acne.
- A daily SPF 30+, broad-spectrum sunscreen – when applied in the morning, this reduces the appearance of dark or light spots on the skin from prior acne and lessens sun sensitivity from certain acne treatments.
- Prescription-strength retinoids – for more advanced or persistent acne breakouts, you may want to work with a dermatologist to receive a prescription for a topical retinoid.
- Other prescription treatments – Your dermatologist may also consider other treatments including but not limited to topical or oral antibiotics, hormonal agents, and isotretinoin depending on the type and severity of acne. More information about the best treatments for certain types of acne can be found above.
In-Office Treatments
As part of their acne treatment regimens, patients may want to consider procedural acne treatment options like:
- Chemical peels – help improve acne by removing dead skin cells, unclogging pores, and promoting smoother, clearer skin.
- Laser and light therapy – often complement other acne treatments by reducing bacteria and inflammation.
- Corticosteroid injections – used to quickly shrink painful cysts and nodules.
Combining Treatments for Best Results
According to Dr. Clarke, “Like most dermatologists, I recommend a multi-phase approach to acne treatment. It starts with developing an effective daily skincare routine and good skin hygiene. From there, I often prescribe topical washes, topical antibiotics, and topical retinoids for mild to moderate acne. In more severe cases, I may prescribe oral antibiotics, isotretinoin, or hormonal therapies. Depending on the patient, chemical peels, laser, and other in-office procedures can also be considered. I work together with my patients to develop the right plan for achieving and maintaining clear skin.”
Lifestyle & Skincare Tips
In addition to at-home and dermatologic treatments for acne, there are some lifestyle and skincare adjustments that those with acne-prone skin can make, including:
- Cleanse properly – washing the skin twice a day with a mild cleanser to clear pores without causing dryness. Avoid harsh cleansers or abrasive exfoliants that irritate the skin, and don’t clean skin too often, or it may damage the skin’s protective barrier.
- Moisturize – skipping moisturizer can dry out the skin and disrupt its natural barrier, which may make oiliness and breakouts worse. Using a lightweight, non-comedogenic moisturizer helps balance hydration without clogging pores.
- Find acne-friendly products – look for cosmetics and skincare products that won’t clog pores. Labels may say things like “oil-free” or “non-comedogenic.”
- Manage stress – elevated stress releases the hormone cortisol that can trigger acne breakouts.
- Dietary changes – some studies suggest that limiting high-glycemic foods and dairy may help some people with acne.
- Avoid picking or popping acne – this can increase the risk of infection and permanent scarring.
Schedule a Dermatologic Visit
If you’re struggling to manage acne with over-the-counter products or you’re dealing with more severe acne, it’s time to consult with a professional. Take just a few moments to fill out the online scheduling request form to get started working with a board-certified dermatologist at U.S. Dermatology Partners. Curious about what skincare products are available to manage acne? Take some time to learn more about the dermatologist-recommended acne solutions available from DermSkincare.
Find a location near me
or