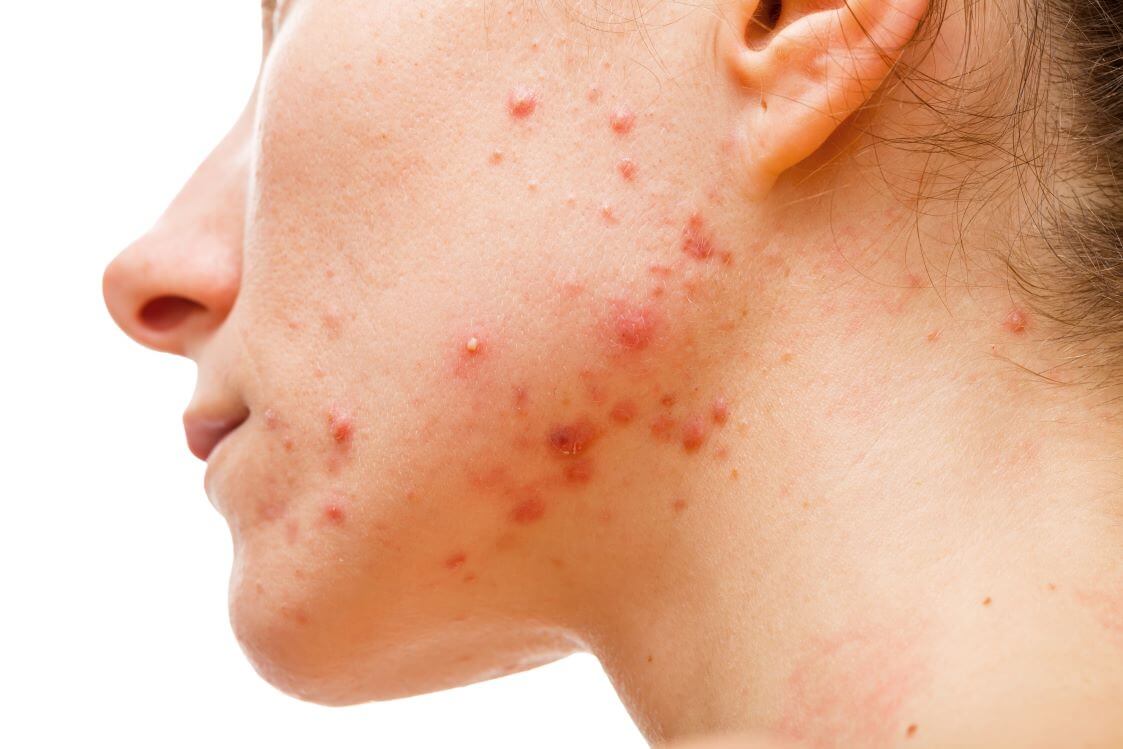
Acne is one of the most common skincare concerns impacting both teens and adults. While most people think of severe acne when they hear that word, there are actually many types of acne that vary in severity. According to Dr. Christina Harview, a Board-Certified Dermatologist with Medical Dermatology Specialists, an affiliate of U.S. Dermatology Partners in Phoenix, Arizona, “Acne is different for every person and even every breakout. To guide our treatment recommendations, dermatologists recognize many different types of acne. The types of acne can also overlap and will vary slightly from person to person, but understanding the basic symptoms of each type can help individuals to find the right options to treat acne.” In this blog, Dr. Harview reviews the basic details of the types of acne and the best treatment options.
Acne 101
Acne is a common, chronic skin condition. It is caused when the body’s natural sebum (oil), which helps to keep skin hydrated, is over-produced, causing dirt, grime, and dead skin cells to get trapped in pores and hair follicles, creating a blemish or pimple. Bacteria trapped within the clogged pore causes acne flare-ups to become inflamed and painful. As pores become more inflamed, bacteria can spread outside the inflamed pore and cause more blemishes to develop. When it comes to the origins of acne breakouts, Dr. Harview says, “Over-production of sebum often occurs for adolescents because changes in hormone levels lead to increased oil production. For most teens and even adults who develop acne, the acne begins as mild, but in some people, it can quickly become severe and require advanced interventions to prevent permanent scarring and maintain healthier skin on a daily basis.”
While pimples are often thought of as only one thing, several types of acne can make up a breakout, including:
- Closed comedones – Commonly referred to as whiteheads, this non-inflammatory form of acne occurs when pores are clogged beneath a layer of skin.
- Open comedones – Commonly referred to as blackheads, this is another non-inflammatory form of acne that occurs when the pores open and become clogged with oil, dirt, and grime. When the sebum and other oils are exposed to air, they are oxidized, which is what turns them black.
- Acneiform papules – In most cases, papules look like small, red blemishes on the skin. They may be painful, especially when touched, but they aren’t always linked to inflammatory acne.
- Acneiform pustules – When papules do not clear up, they may become pustules. These are pimples that may seep pus or produce a discharge if squeezed.
- Nodules – This is the first severe type of inflamed acne. They are large, hard bumps on the skin that can ache even without being touched. They will typically not contain pus or pop when squeezed as the inflammation is present deep within the skin. If squeezed, this infection could spread under the skin, causing a cluster of nodules.
- Cysts – These are large, inflamed lesions filled with pus that occur deep within the skin’s layers. Cystic acne is the most severe form of inflammatory acne. Cysts should never be popped by anyone other than a dermatologist as they may spread, cause infection, and have the highest chance of developing scars.
In addition to the different types of blemishes, there are also four stages of acne severity that will be described in this blog. It’s important to keep in mind that the best option is always to work with a dermatologist to develop a treatment plan personalized to you and your specific skin health needs as these stages are very general and not always adequate to determine the right treatment option. However, being aware of the symptoms associated with each stage of acne can help you better describe your situation and skin care needs to your dermatologist.
Stage 1 – Non-Inflammatory Acne
Non-inflammatory acne typically includes periodic breakouts that consist of mainly opened and closed comedones with a few, infrequent papules and pustules. This type of acne mostly impacts the face, rarely spreading to the neck, chest, shoulders, and back. For people with non-inflammatory acne, the use of non-comedogenic skincare products combined with a targeted treatment plan and medicated acne products during breakouts should be adequate to address flare-ups. According to Dr. Harview, “For mild acne, the key to clearing up breakouts and preventing future acne flare-ups is exfoliation to remove dead skin cells and decreasing oil production or removing excess oil. This can usually be achieved in the early stages of acne breakouts with a few tweaks to the daily skincare routine, including changing exfoliants or exfoliating more frequently. I usually recommend reviewing all skincare products and cosmetics to eliminate anything that is increasing oiliness. I also often recommend prescription creams such as retinoids that help to reduce oil on the skin.”
Stage 2 – Severe Non-Inflammatory Acne
Severe non-inflammatory acne also includes periodic breakouts with a larger number of blackheads and whiteheads as well as an increase in the number or severity of papules and pustules. Again, breakouts tend to be focused on the face with some spread to connected areas like the neck, chest, shoulders, and back. A good daily skincare routine developed with your dermatologist in combination with targeted treatments for breakouts is recommended to address this condition. Dr. Harview says, “A dermatologist can help find the right prescription or over-the-counter topical medications for more severe acne. Medicated treatments for acne usually contain ingredients like benzoyl peroxide or sulfur. These ingredients are anti-inflammatory and antimicrobial and help to dry out blemishes, kill bacteria, and dissolve dead skin cells. If flare-ups become persistent or pustules and papules are painful, they can direct you toward more advanced treatments like oral or topical antibiotics. For some women, we may also recommend taking hormonal birth control pills or other non-birth control hormonal medications, which can help to address acne related to monthly hormonal shifts.”
Stage 3 – Inflammatory Acne
With Inflammatory acne, there may still be blackheads and whiteheads present, but there will be significantly more papules and pustules. Additionally, there will be nodules and a small number of cysts that develop. Breakouts occur more frequently, and they are more likely to spread to the neck, chest, shoulders, and back. Additionally, breakouts may be more painful, red in color, and sensitive to the touch. In many cases, prescription oral or topical medications may be recommended. Dr. Harview describes some of the commonly recommended prescription treatments for acne, “Antibiotics taken orally or applied directly to the skin may be prescribed for inflammatory acne to address bacteria and help breakout heal more quickly. However, antibiotics aren’t recommended for long-term use since people can become resistant to this treatment. Retinoids may be prescribed to improve symptoms. There is an over-the-counter version of retinoids called retinols. Prescription-strength or over-the-counter, these products are derived from vitamin A. They are used to remove dead skin cells, improve cell turnover, kill bacteria, fight inflammation, and help to clear out pores. Topical retinoids may be recommended during breakouts to more quickly heal and reduce the risk for scarring.”
Stage 4 – Severe Inflammatory Acne
Severe inflammatory acne is characterized by large, inflamed, and sometimes infected nodules and cysts. This form of acne is most likely to cause scarring and hyperpigmentation. It is also the most likely to impact all areas of the body in addition to the face. According to Dr. Harview, “Severe inflammatory acne can lead to chronic or prolonged breakouts, and it is often very resistant to topical treatment. While topical retinoids are usually adequate for stage three inflammatory acne, severe inflammatory acne usually calls for a more aggressive treatment. There is an oral retinoid called isotretinoin that is often referred to by its original brand name, Accutane. This treatment option has side effects and requires close supervision by a professional.”
Interested in Consulting with a Dermatologist About Acne?
If you struggle with acne or other common skin conditions, it’s helpful to work with a dermatologist to develop a skincare routine that will diminish the impact of acne to help keep skin clearer. Additionally, those who struggle with acne should visit a dermatologist at least once each year for a skin exam and to discuss any changes in their skin health or issues they’ve experienced since their last visit. If you’re ready to get started working with our team members, simply take a few moments to fill out our online scheduling request form. When a local dermatology office hears from you, they’ll be in touch to finalize the details
Find a location near me
or