While psoriasis is a relatively common skin condition, many people are unaware that it can involve the scalp. In fact, research from the American Academy of Dermatology indicates that about half of the people who are diagnosed with psoriasis will be impacted by scalp psoriasis. Some people only have scalp psoriasis, but this is less common. According to Dr. John “Jay” Wofford of U.S. Dermatology Partners in Dallas and Plano, Texas, “Scalp psoriasis can be hard to spot, and if cases are mild, people may not immediately recognize it as psoriasis, especially if they haven’t been diagnosed with psoriasis in the past. Like other forms of psoriasis, scalp psoriasis is easier to manage if it’s diagnosed in the early, mild stages, so increasing awareness about the warning signs and symptoms of this condition is important.” Keep reading to learn more about what psoriasis looks like as well as possible treatment and prevention options.
What is Scalp Psoriasis?
Scalp psoriasis is a condition that impacts the health and appearance of the skin as well as affecting the immune system. Scalp psoriasis, like all forms of psoriasis, is not contagious and does not seem to be caused by the same environmental factors for each patient (though some people notice specific triggers connected to flare-ups). Whatever the underlying reason, improper immune system function in people with scalp psoriasis causes skin cells to proliferate at an accelerated rate. This immune system dysfunction causes the thickened patches of skin called plaques that are commonly associated with psoriasis.
Scalp psoriasis is more common in adults than children, but children, especially those diagnosed with other forms of psoriasis, may also develop this condition. Like other forms of psoriasis, scalp psoriasis frequently runs in the family, so if you have one or more family members who suffer from this condition, you should be aware of the symptoms and make sure to let a dermatologist know as soon as you notice any of the common warning signs.
Some factors that may affect the severity of an individual’s psoriasis or may serve as triggers for psoriasis flare-ups include:
- Smoking
- Excessive alcohol consumption
- Obesity
- Elevated stress levels
- Certain viral and bacterial infections
- Compromised immune function
- Deficiency of vitamin D
- Skin injuries
- Certain medications
What are the Symptoms of Scalp Psoriasis?
According to Dr. Wofford, “If you’ve already been diagnosed with psoriasis, you know what you’re looking for. In most cases, the way your psoriasis looks and feels on other parts of your body will be very similar to how scalp psoriasis looks and feels. It’s important to remember that the visible symptoms of psoriasis are often the proverbial tip of the iceberg. If you have severe symptoms of psoriasis on your skin, you are likely also experiencing increased levels of internal inflammation. Specifically, people with scalp psoriasis are at a significantly higher risk for developing psoriatic arthritis, even compared to those who only have psoriasis on other parts of their body. Working with a dermatologist ensures you’re managing flare-ups and minimizing the risk of adverse effects on your whole body.”
Scalp psoriasis ranges from very mild and often overlooked cases to severe and prolonged cases that may impact an individual’s overall health and well-being. You can explore some of the most common symptoms of scalp psoriasis in the proceeding sections, and you should contact your dermatologist for an examination and diagnosis if you notice any of the warning signs discussed in the next sections.
Where Does Scalp Psoriasis Develop?
While psoriasis can impact any part of the body, scalp psoriasis affects the top of the head (scalp), hairline, forehead, ears (inside and outside), and neck. Some people have only small patches or spots on the affected skin, but it can also cover the entire scalp.
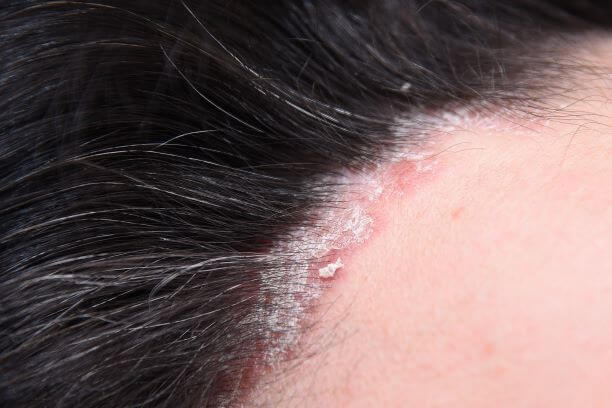
What Does Scalp Psoriasis Look Like?
The appearance of scalp psoriasis varies. If you have psoriasis on other parts of your body, your flare-ups on the scalp will likely look the same. Scalp psoriasis commonly presents with:
- Scaly (thick) patches of skin
- Bumpy patches of skin
- Red or purple skin discoloration
- Thick, silvery-white patches of skin and/or flakes that are like dandruff
- Hair loss (often caused by scratching the skin, not necessarily by the scalp psoriasis itself)
Scalp psoriasis may be confused with another condition called seborrheic dermatitis (dandruff). Like scalp psoriasis, this condition causes itchy and flaky skin. While psoriasis flakes are often dry and white or silver, the seborrheic dermatitis flakes often appear yellow and are greasy.
In some cases, scalp psoriasis is mistaken for dandruff, and if the psoriasis symptoms are mild, the conditions are nearly indistinguishable to the naked eye. It may take a specialist to tell the difference. If you have psoriasis on other parts of your body, it’s much more likely you’re dealing with scalp psoriasis, especially if there are thick patches of skin on your scalp or the condition lasts for weeks without improving.
What Does Scalp Psoriasis Feel Like?
In addition to the way scalp psoriasis impacts the skin’s appearance, you may also experience some or all of the following symptoms:
- Scalp dryness
- Itching
- Burning
- Soreness
Is Scalp Psoriasis Curable?
Dr. Wofford says, “Unfortunately, there is no cure for any form of psoriasis, including scalp psoriasis. However, advancing research has enabled your dermatologist to provide effective treatments to prevent flare-ups and manage symptoms when they do arise. That means most people have mild symptoms that do not last long.”
There is a range of treatments available for scalp psoriasis. In most cases, you’ll begin with medicated shampoos, creams, or other topical treatments that you apply directly to the affected areas. Some of these products (often containing salicylic acid and/or coal tar) are available over the counter and in prescription-strength formulas. Prescription topical treatments may also include ingredients like anthralin, antimicrobials, vitamin D (calcipotriene), corticosteroids, and/or vitamin A derivatives.
For severe symptoms that don’t improve with topical treatment, a combination of in-office and at-home dermatology treatments may be recommended in addition to continuing topical treatments. Some commonly recommended solutions include:
- Laser therapy – using low-heat lasers to address itch and redness and improve scalp psoriasis symptoms
- Phototherapy – using targeted UV light rays to treat the entire scalp, addressing inflammation and itching
- Oral medications – corticosteroids, cyclosporine, methotrexate, retinoids (Vitamin A derivatives), apremilast
- Biologics – adalimumab, brodalumab, certolizumab, etanercept, guselkumab, infliximab, ixekizumab, risankizumab, secukinumab, tildrakizumab, ustekinumab
Can I Prevent Flare-ups in Scalp Psoriasis?
According to Dr. Wofford, “Prevention is an essential part of your scalp psoriasis treatment plan. Each patient will have different triggers that may lead to flare-ups, so the first step toward preventing scalp psoriasis is learning these triggers. I encourage my patients to take a few minutes to note their skin condition as well as any external factors that may have triggered a flare-up. So, patients should make a note of the day, when/how they noticed the symptoms, severity of the flare-up, weather, activities, and other factors that may impact skin health. By tracking these details during flare-ups, patients can begin to recognize contributing factors and avoid potential triggers.”
If you notice scalp psoriasis symptoms, you can also take some steps to reduce the severity of your flare-up. First and foremost, avoid scratching or peeling your flaking skin. This can cause irritation, inflammation, wounds that may lead to infection, and hair loss. Instead, massage the scalp while washing your hair. Then, gently comb or brush the clean hair to remove flakes. Using a leave-in conditioner, shea butter, aloe vera, or other moisturizer applied directly to the scalp after cleaning can also help to alleviate symptoms of scalp psoriasis. Colloidal oatmeal baths, frequently recommended to address psoriasis itch on the body, can also help to relieve itching of the scalp.
There are many home remedies that people with scalp psoriasis swear by, including applying apple cider vinegar, baking soda paste, coconut oil, Oregon grape, tea tree oil, witch hazel, capsaicin, and turmeric mixtures to their scalps. Before using these treatments, you should consult with your dermatologist, but if they help your symptoms, they are typically not harmful.
Visit Your Trusted Dermatologist
If you’re struggling with scalp psoriasis or you’re just ready for an annual skin exam, the U.S. Dermatology Partners team is here to help. You can get started planning your visit right away by completing our online scheduling request form. After we receive your appointment request, a team member will be in touch to finalize appointment details.
Find a location near me
or