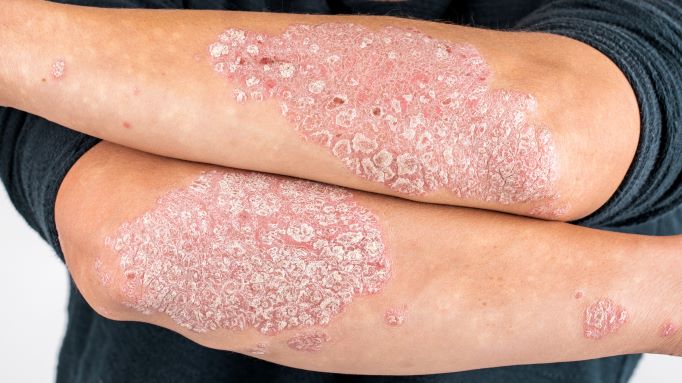
Plaque psoriasis is a chronic condition related to immune system function that results in numerous adverse effects on skin health. According to Dr. Paul Curtiss of U.S. Dermatology Partners in Carrollton, Texas, “Plaque psoriasis is the most common type of psoriasis, impacting as much as 3% of the world’s population, according to the National Psoriasis Foundation. The good news is that means we have done a lot of research and have great support options to help you manage and prevent symptoms of plaque psoriasis.” In this blog, Dr. Curtiss will review just what plaque psoriasis is as well as review prevention and treatment options.
What Is Psoriasis?
When asked about just what psoriasis is, Dr. Curtiss said, “Psoriasis is actually a term that applies to a group of related conditions, including plaque psoriasis, that occurs when the immune system becomes overactive, leading to chronic inflammation, often in the skin. This leads to a range of inflammatory effects, not just in the skin but the entire body. This includes the overproduction of skin cells, itching, and inflammation which visibly manifests as red and scaly plaques, which are often typical of plaque psoriasis. Importantly, psoriasis often co-occurs within both the skin and the joints, in a high proportion of patients. Regular immune function is important to keep the skin and whole body healthy, but overactive immune systems can lead to pain, inflammation, and potentially serious whole-body health concerns. For this reason, it’s important for those who suffer from plaque psoriasis or any other type to create a treatment plan to manage the body’s overactive immune response, which leads to psoriasis flare-ups. While psoriasis can impact any person of any age, it is much more common for adults than children, and it’s significantly more common among those who have one or more close relatives who have this condition.”
What Are the Most Common Symptoms of Plaque Psoriasis?
According to Dr. Curtiss, “Plaque psoriasis is the most common form of psoriasis. When most people think about psoriasis, plaque psoriasis is the type they’re thinking of. Many of the most common symptoms of psoriasis are present in those who are struggling with plaque psoriasis. Specifically, the thick, dry, itchy patches of skin called plaques that give plaque psoriasis its name are the most common symptoms that impact people with psoriasis. Plaque psoriasis is not limited to any one part of the body, but symptoms tend to be most severe on the scalp, back, knees, and elbows. Many patients with psoriasis first develop plaques in these areas, before any other part of the body. Patients may develop psoriasis on many parts of the body, including the trunk, hands and feet, armpit, groin, and genital area. However, I always remind my patients that plaque psoriasis symptoms are more than skin deep. If a patient has severe flare-ups of the skin-related symptoms of their plaque psoriasis, their whole-body health symptoms are also likely to be more severe.”
In addition to plaques, other common signs of plaque psoriasis include:
- Red-colored plaques of skin
- Dry skin with overlying white silvery scale
- Irritated or inflamed skin
- Rashes and itching
- Bumps or lumps on the skin
- Joint pain, stiffness, and inflammation, most often in the early morning
Can Plaque Psoriasis Flareups Be Prevented?
According to Dr. Curtiss, “Flare-ups in plaque psoriasis symptoms are not 100% preventable in every patient. Even those patients who stick to a very strict skincare regimen and take every precaution still may experience increased symptoms periodically. The variety of triggers for plaque psoriasis symptoms is one of the things that makes plaque psoriasis difficult to prevent. As you’re working with a dermatologist to develop a long-term skincare routine to manage symptoms, you should start by pinpointing your specific triggers by tracking flare-ups in your skin condition and working to determine likely causes. This can include things like exposure to certain medications, food, drinks, clothing, skincare products, cosmetics, weather, and stress. Knowing the factors that contribute to your psoriasis flares can positively impact your ability to prevent or minimize the severity of symptoms.”
In addition to learning triggers that may lead to plaque psoriasis flare-ups, some additional preventive measures to reduce flare-ups include:
- Protect skin during cold weather. Keeping skin warm can help prevent flare-ups, so wear warm layers of clothing and try to avoid prolonged exposure to low temperatures.
- In addition to cold, dry weather and low humidity can also trigger flare-ups. Take steps to keep skin hydrated, including using moisturizers and humidifiers to keep skin healthy.
- Get adequate sun exposure. A small amount of natural sunlight can help modulate the immune system’s activity in the skin and decrease the activity of psoriasis. That said, it’s very important to avoid sunburns, and use sunscreen during prolonged sun exposure, which can exacerbate underlying psoriasis
- Avoid skin injuries and treat injured skin right away. Burns, cuts, scrapes, blisters, and even bruises can all contribute to plaque psoriasis flare-ups.
- Make lifestyle changes. Too much stress, poor diet, not enough exercise, and inadequate sleep can all cause psoriasis flare-ups. Make sure you’re maintaining a healthy lifestyle to avoid unnecessary symptom flare-ups.
How Is Plaque Psoriasis Treated? In addition to following these preventive measures, there are several other effective treatment options for plaque psoriasis, including:
- Prescription and over-the-counter cortisone creams may be prescribed to soothe itch and moisturize the skin.
- Vitamin D and retinol creams can significantly improve symptoms during active flare-ups. These are particularly effective when paired with prescription steroid creams
- Ultraviolet light treatments may alleviate the effects of plaque psoriasis, minimizing the impact of flare-ups on the skin for less severe symptoms with a shorter duration.
Many patients who do not improve with the above, may benefit from biologic medications which are often highly effective at both treating active psoriasis and preventing flares.
When Should I Consult with a Dermatologist?
The majority of patients with psoriasis should work with a dermatologist to create a plan that controls symptoms and prevents flares. A dermatologist may also screen patients for psoriatic arthritis, which commonly occurs with psoriasis, and can cause permanent joint damage. Depending on your severity, patients will benefit from at least yearly checkups to ensure treatments are working well and keeping flare-ups to a minimum.
Contact Us for Psoriasis Treatment
If you need to get started, the U.S. Dermatology Partners team would love to hear from you. Our knowledgeable dermatologists can provide the necessary support to minimize the number and severity of plaque psoriasis flare-ups, heal skin during flare-ups, and maintain healthy, beautiful skin. When you’re ready to get in touch with the U.S. Dermatology Partners team, simply take a few minutes to complete our online scheduling request form. We look forward to hearing from you.
Find a location near me
or