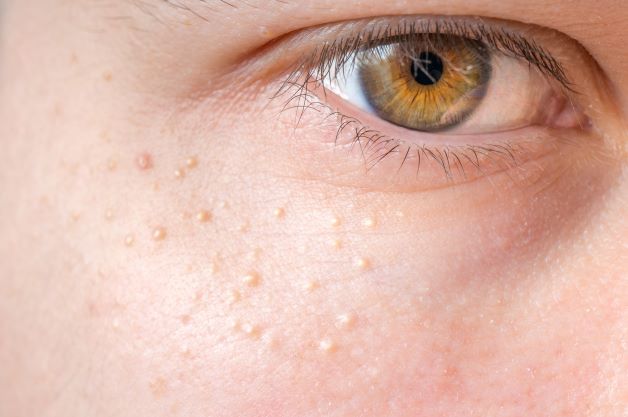
Milia can refer to either a common skin condition or the tiny bumps that are the most common symptom of this condition. According to Dr. Cuong Le of U.S. Dermatology Partners in Centreville, Virginia, “Milia is a harmless but irritating skin health concern that can occur at any age from infancy through adulthood. This condition develops when dead skin cells are trapped below healthy new skin cells because they aren’t removed through exfoliating or shed naturally. Trapped beneath the skin, the keratin in the skin cells hardens, creating small, white or yellow cysts called milia. A single milia is called a milium, but in most cases, milia appear in clusters on the face.” Think you may be dealing with milia? Keep reading to learn more about exactly what milia is and how it’s treated.
What Causes Milia?
When it comes to the causes of milia, Dr. Le says, “There are several different types of milia that have different causes, but regardless of the type of milia, the main underlying cause is the retention of skin cells or diminished skin cell turnover. When dead skin cells aren’t removed quickly enough, they can be trapped beneath the skin. The main difference between something like a pimple or cyst and milia is that the keratin in the trapped skin cells builds up and can harden, creating a firm bump.”
There are six types of milia and each has different underlying causes:
- Neonatal milia – Also called milk spots, this is the most common type of milia and it impacts about 50% of infants. It occurs because infants don’t have fully developed sweat glands, leading to dead skin cells being more likely to be trapped beneath the skin.
- Juvenile milia – This type of milia is less common, and it usually develops as a symptom of other conditions, including Bazex-Dupre Christol Syndrome, Gardner Syndrome, nevoid basal cell carcinoma syndrome, or pachyonychia congenita.
- Primary milia – This type develops due to a buildup of keratin below the skin usually on the eyelids, cheeks, and nose. It is not a symptom of another skin condition. Instead, it is the primary skin health concern.
- Secondary milia – This form of milia develops as a secondary symptom related to other skin health concerns, including infections, injuries, burns, blisters, and rashes. When the skin is damaged, pores are more susceptible to becoming clogged, which in turn can lead to milia forming.
- Milia en Plaque – This is a rare form of milia that most often impacts middle-aged women. It is a secondary form of milia that usually develops as a side effect of autoimmune disorders.
- Multiple eruptive milia – Another rare form of milia, but this one is the most likely to cause serious skin health concerns. In most cases, when milia develop on the body rather than the face, it is multiple eruptive milia. Unlike other forms of milia that develop and clear up relatively quickly, multiple eruptive milia can develop and spread for weeks or even months, and the resulting milia may be painful or itchy.
Who Develops Milia?
According to Dr. Le, “While anyone of any age can develop milia, there are certain factors that significantly increase risk. Some of the most common risk factors include a family history of milia or genetic disorders with milia, as a side effect of oral or topical corticosteroid usage, failure to exfoliate regularly, and using oil-based cosmetics or skincare products. Additionally, some lifestyle factors can make you more likely to develop milia, including using a washcloth, lack of sleep or poor-quality sleep, dehydration, and failure to consume a nutrient-rich diet.”
Can it Be Prevented?
If you are at risk of developing milia, there are some steps you can take to diminish your chances of developing this condition, including:
- Keep skin clean by using a gentle cleanser at least twice a day and any time your skin gets sweaty or oily.
- Exfoliate several times a week, using an exfoliating cleanser or chemical peel.
- Use retinol every night or every other night to promote healthy skin cell turnover.
- Steam the affected areas. This can be done by running a warm bath or shower and sitting in the steam if you have milia affecting the whole body. Place hot water in a bowl and position your face over it with a towel on the head to steam the face. Use caution to avoid burns.
- Apply sunscreen every day to avoid sun damage that can increase your risk of developing secondary milia. A great option that works for most skin types is the SkinCeuticals Physical Fusion UV Defense SPF 50. This physical sunblock is broad-spectrum, meaning it protects against UVA and UVB rays, and the oil-free, lightweight formula works on all skin types, including sensitive, aging, and acneic skin.
What Are the Most Common Symptoms of Milia?
The most common symptom of milia is the development of milia cysts. These small, firm bumps are white or yellow in color. They may be described as feeling like small seeds trapped below the skin. These cysts (unless developed as a symptom of multiple eruptive milia) do not usually cause pain, itch, or create other symptoms.
How Is it Treated?
When it comes to treatment, Dr. Le says, “In most cases, with proper care, milia will clear up on its own. In infants, milia usually clear up and don’t recur. In children, teens, and adults, this condition may flare up more frequently and take longer to clear up. Depending on the type of milia, receiving treatment to clear the current flare-up and developing an ongoing skincare routine is usually all it takes to keep skin healthy. The most important thing to remember is that milia aren’t pimples. They are small, hardened cysts that should not be popped.”
For infants and adults with primary milia, the best course of action may be to allow the skin condition to clear up on its own. However, for milia that are painful, developing in uncomfortable locations, or significantly impacting appearance, there are some treatment steps you can take at home and with the help of a dermatologist to clear a milia flare-up, including:
- Chemical peels – Either in-office or at home, chemical peels can help to reduce the symptoms of primary milia. However, chemical peels can cause secondary milia symptoms to worsen, so consult with a dermatologist before incorporating chemical peels into your skincare routine.
- Retinol spot treatments – These higher concentration retinols are applied only to the area of skin where milia develop. They can help to remove dead skin cells and diminish the appearance of milia. In some cases, tretinoin, a higher-dosage topical retinoid may be prescribed. This is usually reserved to address milia en plaque.
- Comedone extraction – A dermatologist can use a specialized tool to remove the milia cysts.
- Dermabrasion – A dermatologist uses a specialized instrument to remove the outer layers of skin and jump-start the body’s natural healing processes.
- Cryotherapy – This treatment uses cold to freeze cysts.
- Curettage and cautery – This treatment uses heat to remove cysts.
- Laser therapy – This treatment destroys the keratinized cyst and resurfaces the skin.
- Oral antibiotics – These may be prescribed for treating milia en plaque.
When Should I Consult a Dermatologist?
You should consult a dermatologist if milia don’t clear up quickly, they become painful or spread, or milia flare-ups happen frequently. A dermatologist can help you to address symptoms to reduce the severity or longevity of a milia flare-up. They can also partner with you to develop a skincare routine to prevent future milia flare-ups. If you’re interested in working with a dermatologist to address milia or any other skin health condition, U.S. Dermatology Partners would love to hear from you. Getting started is quick and easy. Simply take a few moments to complete our online scheduling request form. Once we receive your request, a local dermatology team member will be in touch soon to answer your questions and set up your first visit.
Find a location near me
or