Keratosis pilaris, or KP, is a common, chronic skin condition. It impacts infants, children, and adults of all ages, and while it doesn’t look or feel great, the good news is that KP typically doesn’t adversely impact skin or overall health. According to Dr. Stephen Matlock of U.S. Dermatology Partners Joplin, Missouri, “Between 40 and 80% of people will be diagnosed with keratosis pilaris in their lifetime. Even though this skin condition is common, there is no cure for it. Instead, individuals who struggle with KP should partner with a dermatologist to develop a plan to alleviate symptoms and reduce the number and severity of flare-ups.” Keep reading to learn more from Dr. Matlock about how to get rid of keratosis pilaris during a flare-up and what steps you can take to improve skin health.
What Is Keratosis Pilaris?
According to Dr. Matlock, “In the name, keratosis pilaris, the word keratosis refers to the underlying cause of KP, which is keratinization of skin cells. Keratinization occurs due to an excessive buildup of keratin, the protein produced in the skin cells, causing the cells to harden usually around hair follicles. Corns and calluses are two other common forms of keratinization. This process is also referred to as cornification, and the resulting hardened and raised skin around the hair follicles can sometimes resemble plucked chicken skin.”
Anyone can develop KP, and it impacts all races and genders equally, but KP does occur more commonly in individuals with eczema and sensitive skin. Infants, children, teens, and adults can all develop this skin condition, but it’s most common in children and adolescents. Many young people who develop this skin condition grow out of it over time, but others can live with it throughout their lifetime. There is no one specific underlying cause of KP, but there are a few factors that increase the risk for KP, including:
- Genetics – Many people who develop this condition have one or more family members who also have KP.
- Chronic skin conditions – Those with dry skin, especially related to skin health concerns like xerosis or atopic dermatitis, are much more likely to develop KP. Additionally, people may develop KP seasonally during the fall and winter months when the weather is cold and dry.
- Health diagnoses – Whole body health concerns like allergies and asthma may increase the risk of developing KP.
What Are the Symptoms of Keratosis Pilaris?
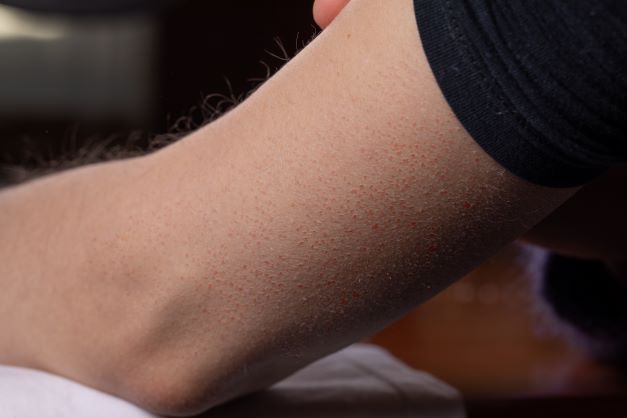
Describing symptoms of keratosis pilaris, Dr. Matlock says, “This condition typically develops as clusters of small, hard bumps that may be red, white, or close to the natural skin tone. KP bumps most often develop on the arms and thighs. In small children, it can also develop on the face and trunk. In addition to the telltale bumps of KP, patches of dry skin may develop on or around the affected area often leading to itchiness and irritation. The skin may also feel generally rough.”
How Can I Prevent Keratosis Pilaris Flare-ups?
Because KP can’t be cured, Dr. Matlock recommends, “Make an appointment to discuss an ongoing care plan with your dermatologist. The right treatment plan can reduce the severity of flare-ups and help you keep your skin clear. While treatment isn’t usually necessary, developing a preventive skincare plan can make a big difference in the health and appearance of skin.” Some of the simple preventive skincare steps you can take to prevent KP flareups include:
- Gently exfoliate regularly to remove dead skin cells and patches of dry skin. Using a bodywash with a mild exfoliant can be helpful. Harsh, physical exfoliants or scrubbing can injure or irritate the skin, so avoid these products. Another good exfoliating option is to incorporate a keratolytic agent into your skincare routines. Products that contain alpha hydroxyl acid, glycolic acid, lactic acid, or salicylic acid as well as retinols and urea serve as a keratolytic to break down the buildup of excess skin cells and hardened skin cells.
- Take care when removing hair. Shaving, waxing, plucking, and otherwise removing hair in areas with a KP flare-up can prolong skin irritation and inflammation. Be gentle, use fresh blades, and apply adequate shaving cream when shaving. Avoid waxing, plucking, and other hair removal techniques during an active flare-up. If possible, consider laser hair removal or other hair removal treatments to avoid irritating the skin.
- Keeping your skin hydrated is of utmost importance. Apply moisturizer to the face and body at least twice a day to keep skin hydrated and the use of an emollient, such as petrolatum jelly, will help the skin retain moisture. One great option to soothe dry, irritated skin related to KP is EltaMD Moisturizer. This product is formulated for extremely dry skin to deliver a boost of hydration and repair the skin’s natural protective barrier for long-lasting moisture.
- Adjust some lifestyle habits to avoid irritating your skin. This may include taking shorter showers or baths and using cooler water to avoid stripping the skin of moisture. You could also review all skincare, cosmetics, and even cleaning products to ensure you’re using products with mild ingredients suited to sensitive skin.
What Are the Treatment Options for Keratosis Pilaris?
According to Dr. Matlock, “Apart from diagnosing the condition and helping patients develop a skincare routine to reduce KP flare-ups, dermatologists don’t typically need to provide much additional treatment for KP. Keratosis pilaris is mostly a cosmetic issue, so taking steps to prevent flare-ups is usually adequate. If treatment is necessary, it is to address specific, treatment-resistant symptoms during an active flare-up. Whatever treatment or preventive measures patients and dermatologists choose can take several weeks to deliver results. It’s important to continue treating skin and practicing recommended skincare regimens consistently. Many people get frustrated by the lack of immediate results and give up. Even if it doesn’t seem like your KP treatment is delivering the desired results, stick with it because the skin takes time to improve. Consult with a dermatologist if you don’t notice an improvement in skin health after the first two weeks of treatment. It may be necessary to adjust your ongoing care plan.”
If KP symptoms can’t be addressed with improved daily skincare and at-home treatments, there are some prescription topical medications and dermatologic procedures that may be recommended for treating keratosis pilaris, including:
- Prescription-strength corticosteroid creams may be used during flares to soften skin and reduce redness and inflammation.
- Laser and light therapies may be recommended to help with swelling, skin texture irregularities, redness, and inflammation.
- Microdermabrasion can be beneficial to remove the hardened dead skin cells and to jump-start the skin’s natural healing processes.
Should I Visit a Dermatologist for Keratosis Pilaris Treatment?
A dermatologist can be a key resource for those who are working to manage the effects of keratosis pilaris. If you’re struggling to get a flare-up under control or want to partner with a professional to prevent symptoms before they begin, Dr. Matlock and the U.S. Dermatology Partners team would be happy to hear from you. Getting started is easy, simply take a few moments to complete our scheduling request form. Once we receive this request, a member of our team will process it and be in touch to finalize the details of your visit.
Find a location near me
or