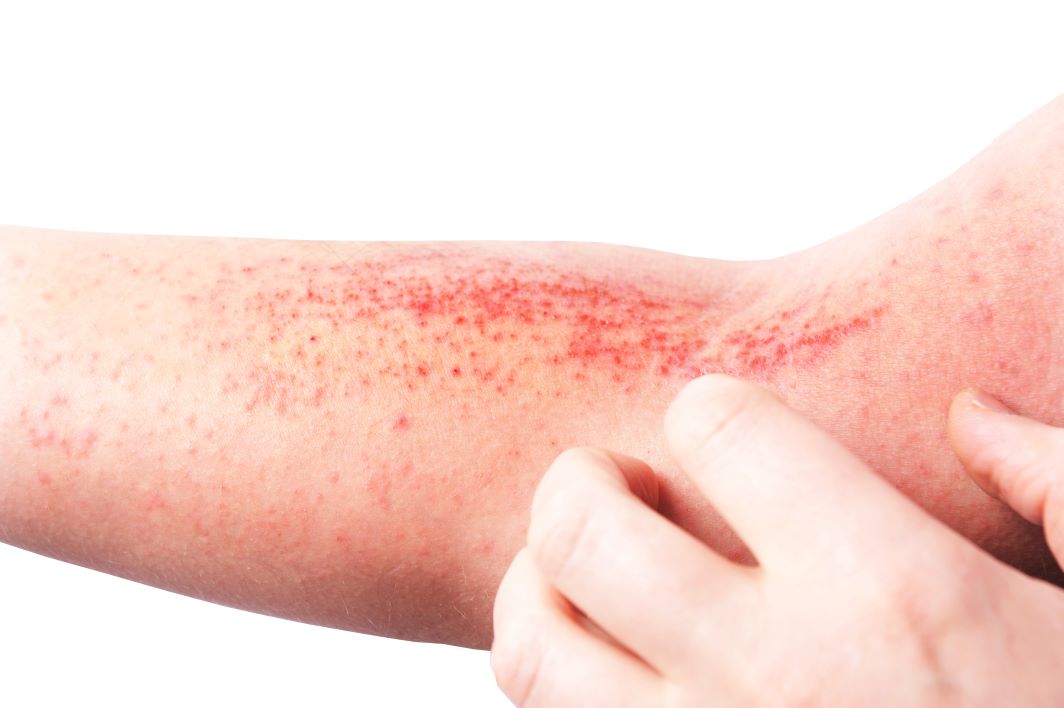
Atopic Dermatitis, more commonly known as eczema, is a common skin condition impacting one in 10 Americans. Millions of people in the U.S. struggle with this condition, and it can impact anyone of any age from infants to aging adults. According to Dr. Lindsay Ackerman of U.S. Dermatology Partners affiliate office Medical Dermatology Specialists in Phoenix, Arizona, “Like other chronic skin conditions, eczema is best managed with the help of a dermatologist. From identifying triggers and creating a customized daily skincare plan to discussing medications and other treatments, a dermatologist can help you achieve and maintain healthy skin.” In this blog, Dr. Ackerman walks through just what atopic dermatitis is, how dermatologists help, available medications an treatments, and at-home care steps.
Introducing Eczema & Atopic Dermatitis
Eczema is an umbrella term that refers to a skin condition wherein there is a breakdown of the skin barrier that causes itchy, red, irritated, and inflamed plaques. While there are several different types of eczema and some varying triggers, what most people think of as “eczema” is actually atopic dermatitis. This form of eczema more commonly first appears in childhood, but it can actually develop at any time. Some of the most common symptoms of atopic dermatitis include:
- Patches of skin that are typically red or brown
- Thickened plaques of skin
- Weeping or painful bumps on the skin
- Itching, burning, or stinging
- Excessive skin dryness
- Skin sensitivity to environmental insults such as hot water, sweating, harsh soaps, and even some creams…. typically those with fragrances or chemical preservatives
- Difficulty falling asleep or staying asleep due to itching or burning
While there is not one underlying cause of eczema, there are some factors that increase risk, including:
- Having an underlying diagnosis of asthma, seasonal allergies (hay fever), or rhinitis
- Younger children with food allergies are more likely to develop eczema
- Genetics plays a role in the development of eczema, as those with one or more close family members with atopic dermatitis are much more likely to develop this condition
The Role of a Dermatologist in Eczema Management
Anyone who struggles with eczema should work with a dermatologist to minimize the signs and symptoms of this condition. Dermatologists can help you identify your triggers, find the safest and most effective skincare products, and understand available treatment options. Dr. Ackerman recommends, “In order to achieve your healthiest skin, you may need to work with a dermatologist over the course of several visits. After you’ve established an effective symptom management plan, you should visit a dermatologist at least once a year for a checkup and to review any medications or other treatments. Even though eczema is a chronic skin condition that doesn’t have a cure, a dermatologist can make the condition more manageable.”
The following are some of the many ways that dermatologists support skin health for those with eczema:
- Alleviate symptoms during a flare-up
- Maintain a healthier barrier function to reduce the frequency and severity of flares with fewer symptoms
- Prevent symptoms from worsening, including decreasing the risk of thickened and itching skin
- Diminished chances of infection (remember, barrier function is key, and without it, you are at risk for both eczema flares and infections in eczema-involved skin)
Eczema Treatment Options: From Topicals to Phototherapy
There are many ways to address eczema, but not all treatments will work for every patient. According to Dr. Ackerman, “Just like every person has different symptoms related to eczema, no two people are predictably 100% the same in their treatment response. In working with a dermatologist, you may need to try a combination of at-home and in-office treatments to achieve and maintain your desired results. There may be some trial and error involved, which can be frustrating. Trust your dermatologist and tell them honestly what is working and what isn’t. They will make adjustments to your treatment plan until your flare-up clears and you can maintain skin health.”
Some common treatments for atopic dermatitis include:
- Topical hydrocortisone creams – These over-the-counter medications help to alleviate itch and reduce inflammation.
- Antibiotic ointments – Sores within eczema may be improved with an over-the-counter or prescription antibiotic ointment. These ointments may be recommended for those at risk for infection. But be careful, some topical OTC antibiotics may actually make eczema worse by causing an allergic reaction. Dermatologists can help you decide what and when it is best to treat with topical antibiotics.
- Wet dressing – Patients who struggle with severe eczema flare-ups may want to consider wet dressings to alleviate symptoms quickly. This treatment involves applying topical medications and then wrapping the impacted area with a damp dressing. Your dermatologist will likely provide this treatment for you first. Then, show you how to replace the dressings at home.
- Phototherapy – Another option for severe eczema flare-ups is light therapy. Using controlled amounts of light applied to the affected area, your dermatologist can help to jumpstart healing and alleviate irritation and inflammation.
Atopic Dermatitis Medication: A Closer Look
In combination with topical medications and treatments, your dermatologist may also recommend prescription and over-the-counter medications. Some of the commonly used medications to manage eczema symptoms include:
- Pain relievers – Acetaminophen and nonsteroidal anti-inflammatory drugs may be used to alleviate discomfort during flare-ups.
- Antihistamines – For those who have seasonal or environmental allergies, managing allergy side effects can help diminish eczema symptoms. Taking a daily antihistamine for allergies can be an essential aspect of many eczema treatment plans.
- Oral corticosteroids – Like topical corticosteroids, these oral medications can help manage eczema symptoms during flare-ups, but are not recommended for chronic use.
- Calcineurin inhibitors – These immunomodulators have been the preferred method of treating eczema for years (this chronic topical application is safe. They reduce the body’s response to allergens and irritants that trigger flare-ups, reducing eczema symptoms.
- Chronic systemic therapies such as Biologics (injections) or small oral molecules (pills) – When people are unresponsive to more conservative eczema treatments, a chronic systemic medication may be most appropriate. These treatments are typically reserved for patients with more severe disease, or those recalcitrant to other conservative treatments.
Lifestyle Adjustments for Eczema Control
In response to how to manage eczema, Dr. Ackerman says, “Learning your triggers and minimizing contact with them is the most important step you can take to prevent eczema flare-ups at home. As part of your work with a dermatologist, you should track any increase in eczema symptoms as well as possible sources of your symptoms. From there, you can work with a dermatologist to make specific adjustments to your daily routine to maintain optimal skin health.”
Some of the other at-home care steps you can take to control eczema flareups include:
- Maintaining a consistent morning and evening skincare routine with products outlined by your dermatologist.
- Using lukewarm instead of hot water and taking shorter showers and baths to limit moisture loss.
- Applying moisturizer right after showering, bathing, and washing your face. This will help you trap moisture and keep your skin hydrated. EltaMD Moisture Seal is a great whole-body option to keep skin hydrated without the risk of irritation.
- Evaluating household cleaning products, cosmetics, and skincare products for dyes, parabens, fragrances, and other ingredients that cause skin irritation or trigger eczema flare-ups. Minimize contact or replace these products with options that are better for sensitive and eczema-prone skin.
- Getting rid of clothing, towels, and bedding made from rough or irritating fabrics and those that don’t breathe like wool, polyester, and nylon. These fabrics may contribute to eczema flare-ups.
Conclusion: The Journey to Better Skin Health
When it comes to the decision to seek treatment for eczema, Dr. Ackerman says, “People can live for years with the negative effects of eczema believing the discomfort, itchiness, and other symptoms are something they just need to put up with. While eczema can’t be cured, your dermatologist will provide treatments, medications, and skincare options that can significantly improve comfort even during flare-ups. With consistent daily skincare and symptom management, you’ll look and feel better quickly.”
Talk to a Professional
If you believe you’re struggling with atopic dermatitis, a dermatologist can help you manage symptoms and minimize discomfort. Working with a knowledgeable professional ensures you’ll have the best chance to avoid flare-ups. When you’re ready to get started, simply take a few minutes to complete our online scheduling request form. Once we hear from you, a local team member will be in touch to finalize the details of your visit.
Find a location near me
or