Though some skin conditions can be treated with over-the-counter lotions, creams and gels, others are more serious — sometimes even life threatening — and need to be evaluated and treated by a board-certified dermatologist.
How can you tell whether your skin condition is serious enough to require professional help? These five signs will help you determine when it’s time to find a dermatologist.
Get your FREE eBook!
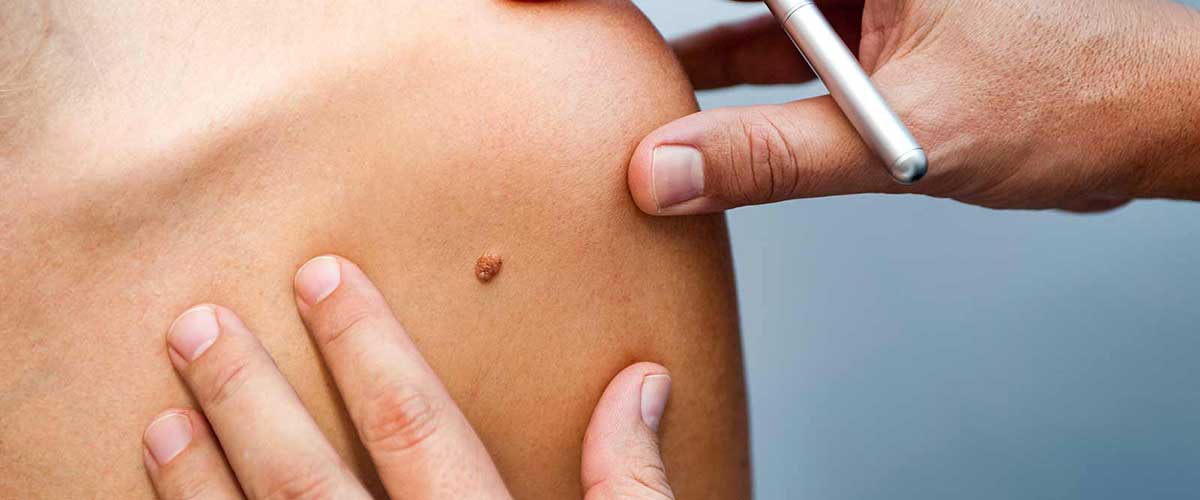
Sign #1: You have a new spot on your skin, a spot that looks different than all of your others or a mole that has changed size, shape or color.
Skin cancer — the most common form of cancer in the U.S. — is the result of the uncontrolled growth of abnormal skin cells. When skin cells suffer DNA damage, they can mutate and multiply quickly to form cancerous (malignant) tumors.
Skin cancer is considered “low risk” when the affected cells stay clustered in a single group. It becomes “high risk” when these abnormal cells invade surrounding tissue.
The good news is that if skin cancer is detected early, before it spreads, chances of a complete recovery are very high.
There are many different types of skin cancer. Most are easy to detect with a skin examination and develop on the skin’s outer layer on areas that are exposed to the most sun. These areas include your face, head, hands, arms and legs. Types of skin cancer include:
Actinic Keratosis
These pre-cancerous lesions develop on sun-exposed areas and can be a warning sign that skin cancer is developing. Generally, the tumors stay contained and don’t spread to other areas.
Basal Cell Carcinoma
This type of cancer typically begins as a small, shiny bump on the face, though it can occur on any part of the body. If caught and treated early, basal cell carcinoma is rarely life threatening. If left untreated, however, it can spread to nearby bone or tissue.
Up to 30% of Caucasians may develop basal cell carcinomas during their lifetime.
Squamous Cell Carcinoma
This cancer develops in the squamous cells that make up the outer layer of skin, typically on areas that are most exposed to the sun. It can show up in many forms — a firm, red nodule; a flat sore with a scaly crust; or a new sore or raised area on an old scar or ulcer. Though rarely life threatening, squamous cell carcinomas can be aggressive and can spread to other parts of the body.
Melanoma
The deadliest form of skin cancer, melanoma can spread very quickly and become life threatening if not diagnosed early. Melanoma can start as a sore that doesn’t heal or as a mole with an irregular border. A mole with redness or swelling beyond its border, one with surface changes or a mole that has associated itchiness, tenderness or pain can also be signs of melanoma.
So, how do you determine if a mole or spot is skin cancer?
In most cases, moles and spots are harmless and come in a wide variety of shapes and sizes. Some moles, however, are not normal and need to be examined by a dermatologist.
Normal vs. Atypical Moles
“Normal” moles are usually smaller than a pencil eraser. They are round and symmetrical with an even color and smooth borders.
Most moles can be classified as flat moles, raised moles or skin tags. Flat moles are generally dark or irregular spots on your skin. Raised moles are deeper than flat moles and can appear in a wide range of colors. Skin tags are just painless growths on the skin — sometimes a shade darker than your primary skin tone.
All of these moles are harmless and do not need to be removed for medical reasons. On the other hand, atypical moles — also called dysplastic nevi — are unusual looking moles that look different than healthy, normal moles when viewed at the cellular level. They are typically asymmetric and very dark or multi-colored. They may have indistinct borders and are most commonly found on the back, chest, buttocks or scalp. Though atypical moles may look like melanoma, they are non-cancerous and won’t necessarily turn into skin cancer. However, if you have atypical moles, you may have a higher risk of developing skin cancer in the future.
Anytime you have a suspicious mole or spot on your skin that looks different than the others on your body — or you have a new mole after age 40 — you should have it checked by a dermatologist.
Look for the ABCDEs:
Asymmetrical – One half doesn’t mirror the other half.
- Border that is ragged – The edges are ragged, irregular or notched.
- Color that is non-uniform – The color is not consistent throughout. Look for different shades of tan, brown or black.
- Imension larger than 6mm – The diameter is roughly ½ inch or larger.
- Evolving appearance – There is a change in the color or an increase in size over time.
Most dysplastic moles will remain stable and don’t need to be removed, but they should still be watched closely at home and monitored for any changes. Your best bet is to screen your skin monthly on your own and see your dermatologist for skin exams every six to 12 months.
Remember to check every part of your skin — even between your toes and on the bottoms of your feet — on a regular basis. If you can’t see a particular part of your body, ask someone you trust to help check your skin. It’s also a good idea to take pictures of abnormal moles as a reference so that you can see if they have changed.
When in doubt, have your dermatologist evaluate any and all areas of concern.
Download Ebook of this content
Sign #2: You Need To Have A Mole Or Skin Cancer Removed.
If you have atypical moles or develop new moles after the age of 40, a dermatologist will most likely want to biopsy one or more of your moles.
If the biopsy shows that the mole is benign, your doctor will likely recommend that you continue to monitor it over time. Otherwise, your doctor may determine that it needs to be removed.
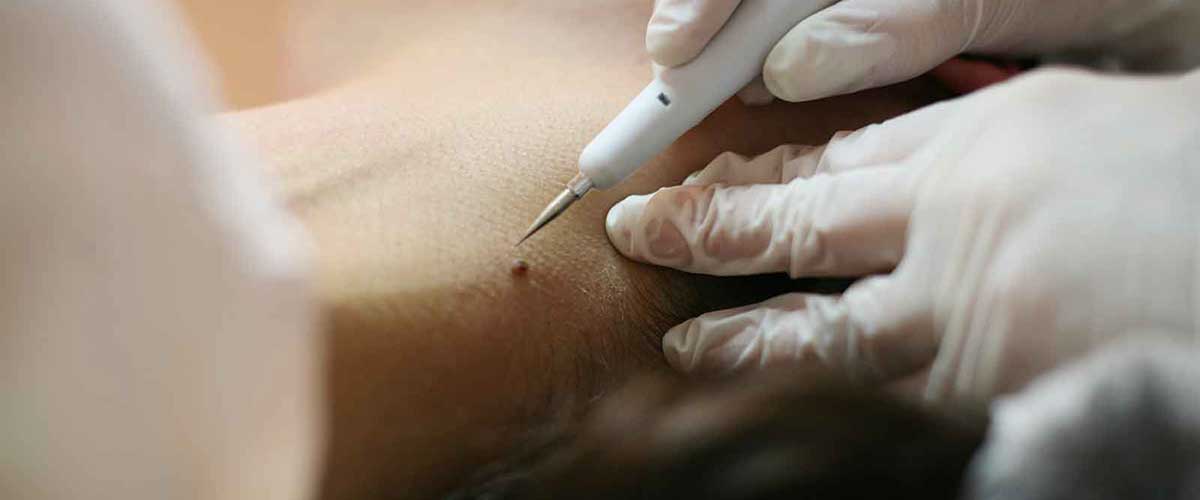
Cryotherapy, or cryosurgery, is a simple, non-invasive procedure that uses liquid nitrogen to freeze and destroy moles and other growths on the skin. By applying liquid nitrogen directly to skin lesions, dermatologists can target damaged skin cells and destroy them at the cellular level.
The procedure is simple, affordable and virtually painless. The affected area may blister and scab over, but should completely heal within three to six weeks.
Skin Cancer Treatments
Cryosurgery can also be used to treat precancerous skin lesions or types of skin cancer where the cancer is still localized and hasn’t spread to other parts of the body.
Other treatments for skin cancer that your dermatologist can perform include:
Mohs Micrographic Surgery
The most effective treatment of squamous cell carcinoma and basal cell carcinoma, the Mohs surgical technique enables your dermatologist to remove skin cancer using precision, microscopic control.
The cancer is removed layer-by-layer and analyzed under a microscope until all cancerous cells are gone. This allows the surgeon to get rid of all of the cancer without damaging surrounding healthy tissue. An added benefit of this technique is that it results in the smallest possible wound.
Surgical Excision
Surgical excision is the removal of skin cancer with a scalpel under local anesthetic. This treatment method is typically very successful because it not only removes the skin cancer, but also some of the surrounding normal skin to ensure the cancer has been completely removed.
Curettage
A common treatment for basal cell and squamous cell cancers, curettage is used to remove skin cancer by scraping the area with a sharp loop-edge instrument called a curette. An electrocautery needle is then used to destroy any remaining cancer cells. The process can be repeated multiple times until all of the cancer cells have been destroyed.
Your doctor will consider many factors before recommending a skin cancer treatment plan that is best for you.
Tips for Preventing Skin Cancer
Protecting your skin from damaging UV rays is your #1 defense against skin cancer. To reduce your chances of developing skin cancer:
- Limit the amount of time you spend outside during peak sun hours (10 a.m. to 4 p.m.).
- Wear a broad-spectrum sunscreen with an SPF of 15 or higher every day.
- Wear protective clothing in the sun (long pants, a long-sleeved shirt, broad-brimmed hat and UV-blocking sunglasses).
- If you’ll be spending an extensive period outside, use a water-resistant, broad-spectrum sunscreen with an SPF of 30 or higher.
- Avoid sunburns and tanning booths.
- Check your skin at home every month and monitor all changes.
- Schedule a professional skin exam with your dermatologist every six to 12 months.
Download Ebook of this content
Sign #3: You Have Severe Acne That Isn’t Responding To Over-The-Counter Medications.
Acne is more than just a cosmetic problem — it’s a serious dermatological condition caused by inflammation in pores that have been clogged with oil, dead skin cells or bacteria. When pores get clogged, the bacteria inside multiplies and causes your immune system to react with swelling and redness, forming a “pimple.”
Acne affects men and women of all ages and can be triggered by hormones, diet, stress and even some medications.
Mild forms of acne can sometimes be treated with over-the-counter products, but if you have stubborn, recurrent acne that is not clearing up after months of using these treatments, it’s time to find a dermatologist.
What Is Cystic Acne?
Cystic acne is a severe form of acne that occurs when oil and dead skin cells build up in pores and rupture. The inflammation extends deep into your skin, forming a tender red bump that is often filled with pus. If the cysts burst, the inflammation can spread and lead to more breakouts or even scarring.
Cystic acne won’t go away on its own and won’t respond to over-the-counter medications. You can’t take care of it by excessively scrubbing your skin or squeezing blemishes. In fact, these methods can cause the infection to deepen and ultimately make the situation worse.
Cystic acne needs to be treated by a board-certified dermatologist.
Acne Treatments
Your dermatologist might recommend one or more of the following treatments to clear your recurrent or cystic acne:
Topical Treatments
Prescription-strength topical creams and gels that include benzoyl peroxide and retinoids can effectively unplug pores, kill bacteria and reduce inflammation. Retinoids like tretinoin (Retin-A, Differin and Tazorac), adapalene and tazarotene are all topical drugs designed to prevent hair follicles from becoming plugged.
Oral Antibiotics
Oral tetracyclines such as minocycline and doxycycline can also help reduce inflammation and control the growth of bacteria.
Accutane (Isotretinoin)
This powerful drug (and its generic counterparts Amnesteem, Claravis and Sotret) works by reducing the amount of oil released by oil glands in the skin. For most people, a single dose taken once or twice daily for five months clears the skin completely and permanently.
Hormonal Treatments
Oral contraceptives that combine estrogen and progestin can be used to treat acne in some women.
Chemical Peels and Laser Therapy
If you have had severe acne in the past that has led to scarring, there are many non-surgical treatments available to help improve the appearance of your skin. Chemical peels, microdermabrasion and laser skin resurfacing can all reduce the appearance of scars and improve your skin’s surface.
Be sure to discuss the risks and side effects with your doctor before starting a new treatment plan.
Preventing Acne:
In addition to the medical treatments for cystic acne, there are also several lifestyle changes you can make to improve your condition:
- Avoid high-glycemic foods such as ice cream, soda, candy, potato chips, white bread and other processed foods and sweets.
- Eat more whole foods such as whole grains, vegetables, beans and fruits.
- Cut back on the dairy. Substitute almond or coconut milk for cow’s milk.
- Lower your stress.
- Don’t try to “pop” pimples and cysts. That only makes acne worse!
Download Ebook of this content
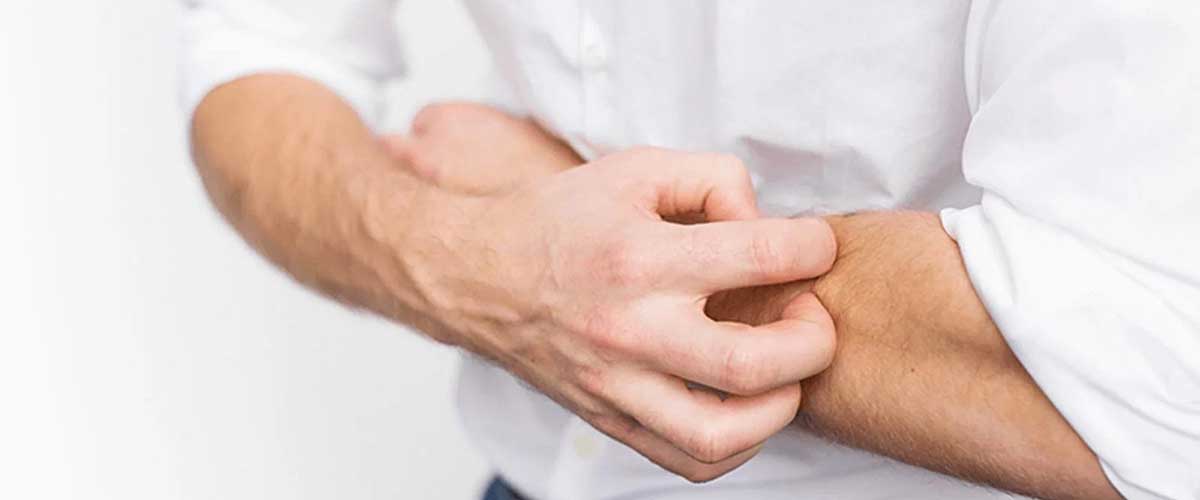
Sign #4: You Have Persistent Itching Or A Rash That Won’t Go Away.
There are several skin conditions that can cause uncomfortable inflammation, itching and flaking skin that just won’t clear up on their own. If you have a rash or persistent irritation and itching, it might be time to ask your doctor for help.
Eczema
Also called dermatitis, eczema is a common condition with symptoms that can range from mild itching and redness to severe scaling and cracking of the skin. Causes can include genetics, age, allergies or an overactive immune system.
Psoriasis
Psoriasis — a chronic autoimmune inflammatory condition — causes patches of skin to become inflamed, red and bumpy. This occurs when the immune system mistakes skin cells for a virus or other infection and responds by producing more skin growth.
Rosacea
A fairly common skin condition, rosacea causes redness in the face and sometimes small, red pus-filled bumps or swollen blood vessels on the nose and cheeks. Symptoms can last for weeks or months at a time and can sometimes be mistaken for acne or other skin conditions.
In most cases, your dermatologist can prescribe oral or topical medications — and even some laser therapies — to help ease the symptoms of these skin conditions.
Download Ebook of this content
Sign #5: Your Appearance Is Damaging Your Confidence Or Negatively Impacting Your Quality Of Life.
There are many symptoms and medical conditions that require a dermatologist’s immediate attention, but your doctor can also help with a number of cosmetic concerns.
In addition to medically treating skin conditions, dermatologists provide a wide range of minimally invasive, low-impact cosmetic treatments to restore your skin’s youthful appearance and help you regain your self-esteem and confidence.
As we age, our appearance changes in many ways that can affect our overall wellbeing. Skin loses its elasticity and collagen. Wrinkles appear on the face after years of repetitive expressions. Hair begins to thin and fall out where we want it and grow where we don’t want it. These changes can cause emotional distress and can even lead to depression.
Cosmetic surgery and non-surgical treatments are designed to help you look and feel your best, and most are conducted in your dermatologist’s office with little or no downtime.
Injections and Dermal Fillers
Sometimes called injectable wrinkle fillers, dermal and soft tissue fillers are an affordable way to smooth out the surface of your face. Most procedures can be quickly performed in your dermatologist’s office, and results last for several months.
These treatments include Botox, which works by relaxing the muscle under the wrinkle, as well as injectable dermal and soft tissue fillers that fill creases in the skin with another substance to restore volume.
Fillers can be hyaluronic, synthetic, collagen or even autologous, which means fat from your own body is surgically removed, treated and injected.
Skin Resurfacing and Rejuvenation
In addition to facials and chemical peels, dermatologists offer a number of other treatments to exfoliate, even out the skin’s surface and improve the overall appearance of your skin.
These procedures include CO2 laser restoration, dermaplaning, IPL photo rejuvenation, laser skin resurfacing, laser vein elimination, microdermabrasion, microneedling, platelet-rich plasma (PRP) therapy, skin lightening, tattoo removal and more.
Many of these state-of-the-art, minimally invasive treatments use laser technology and are performed in the comfort of your dermatologist’s office.
Fat Reduction
There are several cosmetic procedures to reduce and destroy fat in your abdomen, thighs, buttocks, neck, chin, upper arms and back. In addition to traditional liposuction, which is designed to “suck” unwanted fat from various parts of the body, these treatments include:
Body Contouring
This non-surgical treatment reduces fat or melts it away with ultrasonic waves and radio frequencies.
Hair Removal and Restoration
Whether you want more hair on your head — or less hair in certain places — there are many procedures available to help improve your appearance and restore your confidence.
In addition to traditional hair restoration methods, non-invasive follicular transplant options are also available. These procedures restore hair naturally without the risk of linear scarring.
Laser hair removal is a medical procedure that uses laser technology to remove unwanted hair, and Latisse is a prescription-only product to help you grow longer, lusher eyelashes.
Surgical Procedures
Your dermatologist can also perform a number of safe, surgical options to help you feel younger and more confident.
Microneedling
This minimally-invasive procedure fills fine lines in the face by stimulating collagen production.
Platelet-Rich Plasma Therapy
PRP Therapy is a method of skin rejuvenation that has also been effective in treating alopecia. After separating plasma from platelets in the patients’ blood, the plasma is re-injected into the face or scalp to encourage cell growth, collagen and tissue regeneration.
When should you call in the professionals?
Call a board-certified dermatologist when:
- You have a new spot on your skin, a spot that looks different than all of your others or a mole that has changed size, shape or color. Monitor your skin monthly at home and if you see something that looks suspicious, call your doctor and have it checked. A board-certified dermatologist can tell you if it needs to be monitored, biopsied or even removed.
- You need to have a mole or skin cancer removed. One in five Americans will develop skin cancer during his or her lifetime. Find a dermatologist and schedule an annual skin cancer screening today.
- You have severe acne that isn’t responding to over-the-counter medications. Your dermatologist can find a treatment plan that is right for you.
- You have persistent itching or a rash that won’t go away. If over-the-counter treatments just aren’t working, it’s time to enlist the help of a professional.
- Your appearance is damaging your self-confidence or negatively impacting your quality of life.And if your appearance is causing you to suffer — if you don’t feel like the person you used to be — talk to your doctor about surgical and non-surgical options to help you recover your self-confidence.