When it comes to caring for your skin, psoriasis is one of the most challenging conditions a person can face. Treating psoriasis can be a real challenge. There are a number of fantastic treatments for psoriasis. However, there isn’t one single best psoriasis treatment. There are different types and severities of psoriasis, and it’s essential that patients partner with a board-certified dermatologist to receive an accurate diagnosis and develop a plan to prevent flareups and address them right away when they do arise. Keep reading to learn a little more about the types and causes of psoriasis and some of the best treatment options.
What is Psoriasis?
Psoriasis is a type of autoimmune disorder. In most cases, psoriasis causes the rapid buildup of skin cells resulting in the development of thick, scaly patches of skin called plaques. As an autoimmune disorder linked to inflammation, psoriasis can also cause swelling and pain in the joints.
Related: How to Manage Psoriasis in Cold Weather
What are the Types & Causes of Psoriasis?
While research still isn’t 100% conclusive about the cause of psoriasis, almost all cases are inherited. If you have a family member who sufferers from psoriasis, you should be aware of the early warning signs of this condition and seek treatment right away. Psoriasis is a genetic disease that causes the body’s immune system to become overactive. It may overreact to an injury, bacteria, virus, or other foreign body. The increase in inflammation caused by psoriasis affects not only the skin but can also cause damage to organs and other health concerns. The external rash tells us a lot about how advanced the condition is, so when you are experiencing a psoriasis flareup, it is essential to address the inflammation as well as the skin plaques. In order to appropriately address psoriasis symptoms, we need to start by accurately diagnosing your psoriasis.
Plaque Psoriasis
This is the most common form of psoriasis, and it is likely what comes to mind when most people hear the word. Plaque psoriasis leads to the buildup of red, raised, thickened areas of skin called “plaques.”
Guttate Psoriasis
Guttate psoriasis is a less common form of the condition that occurs in less than 1/3 of those who suffer from psoriasis. It is most often diagnosed in children and associated with preceding Strep throat infections. It causes small, teardrop-shaped spots on the skin. These spots are typically red or pink in color, and they are most likely to form on the torso, arms, and legs. While the spots that appear from guttate psoriasis aren’t as thick or painful as other forms of plaques, those who are diagnosed with guttate psoriasis may actually suffer from plaque psoriasis and other forms of psoriasis at the same time. In some cases, the flareups on the arms, legs, and torso may start to spread to other parts of the body, including the face.
Inverse Psoriasis
This form of psoriasis does not create the thick, itchy plaques characteristic of psoriasis. For those with inverse psoriasis, the plaques usually develop in the skin’s folds and are flatter with less scale. Areas like the underarms, beneath and between the breasts, and around the genitals and buttocks are most likely to be affected by inverse psoriasis. Because the skin in these areas is thinner and more sensitive, managing inverse psoriasis can be a challenge. Flareups are often very painful, and the folding of the skin may lead to cracks in the skin, called fissures, that expose you to the risk of bacterial, yeast, and/or fungal infections. Inverse psoriasis has been linked to other risk factors, including smoking, obesity, certain medications, chronic infections, and stress. In many cases, we’ll need to address these related risk factors in order to help you achieve healthy, pain-free skin.
Pustular Psoriasis
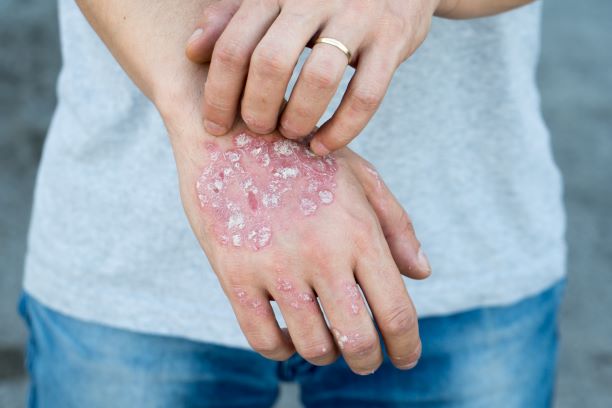
Traditionally, psoriasis is associated with thick, red and pink patches of skin called plaques. Pustular psoriasis flareups can look like traditional psoriasis plaques, but when you look a little closer, you’ll notice there are actually blisters or pus-filled sores (pustules) on the plaques. In most cases, pustular psoriasis flareups are limited to the hands and feet, but they can be on all of the plaques on the body.
Erythrodermic Psoriasis
This is the rarest and most severe form of psoriasis. When flareups occur, over 90% of the skin is covered with redness in addition to the common plaques of psoriasis. Erythrodermic psoriasis patches are so extensive that people with this condition may appear sunburned. In addition to painful, itchy patches covering large parts of the body, erythrodermic psoriasis can lead to high fever and illness. Without proper care, erythrodermic psoriasis can be life-threatening. In many cases, people who develop erythrodermic psoriasis may need hospitalization for treatment and monitoring.
Psoriatic Arthritis
In addition to its impact on the skin, psoriasis also causes inflammation that can impede the healthy function of joints in the body. Psoriatic arthritis causes pain, swelling, and limited joint motion, and it can impact people who suffer from any type of psoriasis.
The Best Treatments for Each Type of Psoriasis
There are many types of psoriasis that impact each person differently, and many people can have multiple types of psoriasis at once. Your dermatologist will want to work with you to develop a personalized plan to address the specific symptoms related to your psoriasis. If you’re experiencing inflammation, chronic infection, or other related conditions, we’ll also want to address these as part of your psoriasis treatment plan. The good news is that the treatment of all types of psoriasis has progressed significantly in the past two decades. If managed properly in partnership with a knowledgeable, board-certified dermatologist, most people can achieve 90% to 100% clearance. No one should have to live with psoriasis.” Some of the most effective treatments for each of the types of psoriasis are listed below.
Plaque Psoriasis
There is no cure for any type of psoriasis, so the goal of treatment is always to clear skin psoriasis and prevent flareups whenever possible. For plaque psoriasis, we will start by trying to track the potential triggers and limit your exposure to conditions that can lead to a flareup. If the patient has relatively few plaques, we’ll likely start with a topical medication to fade away the psoriasis plaques. For wider spread plaques, we may recommend starting with a round of light therapy in our office. These light systems may also be available for at-home use. For more severe cases, we may prescribe medications that target certain parts of the immune system to help alleviate symptoms. These medications are available as pills or injections.
Guttate Psoriasis
Unlike other types of psoriasis that have chronic and long-lasting breakouts, guttate psoriasis is not necessarily a chronic condition. If treated early and appropriately, it can clear quickly and never recur. For most patients, we may use light therapy and prescribe systemic medications. Additionally, if a patient has Strep throat when they get this breakout, we must be certain that the Strep throat was treated adequately in order to help fully clear the psoriasis breakout. For some patients, a guttate psoriasis flare may be the first presentation of your chronic psoriasis, so seeing a board-certified dermatologist in order to properly manage your psoriasis is very important.
Inverse Psoriasis
In most cases, treatment for inverse psoriasis will include topical corticosteroids. We may also prescribe medications specifically to target the yeast, fungal, and bacterial infections that are commonly associated with this condition. Light therapy is also commonly used. Finally, medications that slow the replication of skin cells may also be prescribed.
Pustular Psoriasis
Pustular psoriasis happens either on the palms of the hands and soles of the feet, or it is associated with the normal psoriasis plaques on the skin. This form of psoriasis is one of the most difficult forms of psoriasis to treat. Treatments can include topical or systemic medications used in combination. Some may even use light therapies. Your doctor may also address other potential causes of your pustular psoriasis, including smoking.
Erythrodermic Psoriasis
This is a very serious condition that can be life-threatening, so if you have warning signs of this condition, you should seek medical help right away. Depending on the severity of your condition, you may be prescribed a combination of medications that can include any of the following:
- Cyclosporine – and similar medications used to stop the immune attack
- Methotrexate – and similar medications to control cell growth
- Adalimumab – or other medications to suppress the overactive immune system
We may also prescribe antibiotics, pain medications, and medications to help with itching. In addition to these medications, you may also receive topical creams or ointments. Wet wraps and oatmeal baths can also help to soothe the skin.
Psoriatic Arthritis
For those who have psoriasis and may be experiencing joint symptoms of psoriatic arthritis, it is important to be seen by a Rheumatologist. Your Dermatologist and Rheumatologist will typically work together to form a good treatment plan for you to address both your skin and joint symptoms.
Related: What Our Experts Are Saying About Biologics for Psoriasis
The Importance of Partnering with a Dermatologist for Psoriasis Treatment
Because psoriasis can affect people in so many ways and because there are a range of treatments available for use, working with a board-certified dermatologist to find the right psoriasis treatment is essential. If you have been diagnosed with psoriasis or suspect you may be developing this condition, you should find a dermatologist to support you in maintaining healthy skin. There are numerous U.S. Dermatology Partners locations, so get started by completing our online request form. The office closest to you will be in touch soon to confirm your visit.
Find a location near me
or