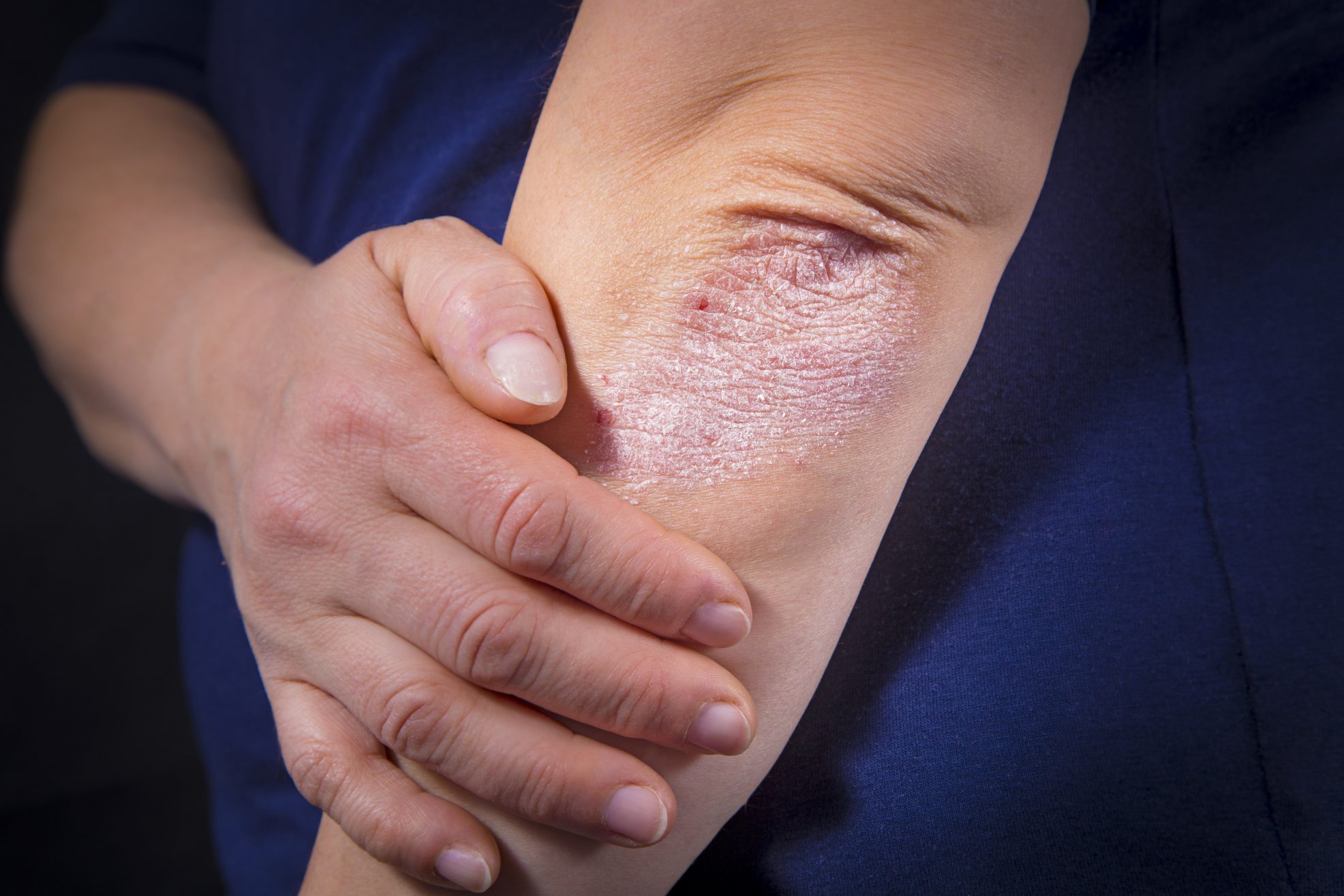
Psoriasis is a common autoimmune disease that often presents as a severe skin condition, and it can affect almost anyone. There are many assumptions people make about this common condition, and they are not necessarily accurate. We invite you to discover the truth behind seven of the common myths people believe about psoriasis.
Myth #1 Psoriasis is Only Skin Deep
Many people believe that psoriasis is just dry, scaly skin, but it’s actually an autoimmune disease. This condition causes the immune system to malfunction and produces new skin cells too quickly. With the cells being produced so rapidly, they don’t shed quickly enough, which leads to the patchy, red areas of skin that are often indicative of psoriasis.
In addition to the way psoriasis affects your skin, there are other symptoms you should be aware of. The most common is pain or itching around the patches of skin. The skin patches can also crack and bleed putting you at risk for infection. Because psoriasis originates in the immune system, it is also connected with health conditions like diabetes, heart disease, and arthritis.
Because of the impact psoriasis has on the appearance, many people who struggle with this condition also deal with stigma from their peers and coworkers, putting a strain on developing personal and professional relationships. People who have psoriasis often struggle with depression, and they may be more likely to consider, attempt, or commit suicide.
Myth #2 Psoriasis is Contagious
You cannot catch psoriasis or give it to anyone else! Sharing food, clothes, hugging, kissing, and even sexual contact cannot spread psoriasis. The belief that psoriasis is contagious leads to much of the stigma surrounding this disease.
Myth #3 Psoriasis can be Cured
Unfortunately, psoriasis cannot be cured, but in most cases, it can be managed with customized treatment plans. Even those with well-managed psoriasis will still have periods of flareup throughout their lifetime.
In order to treat psoriasis, your dermatologist or physician will want to address three issues: the overproduction of skin cells, the skin itching, inflammation, and irritation, and the removal of dead skin. Your treatment plan will be unique to your needs and may include a combination of oral, topical, or injected medications, light therapies, and other skin treatments.
Related: Biologics for Psoriasis
Myth #4 All Psoriasis is the Same
There are a number of different forms of psoriasis, including plaque, guttate, inverse, pustular, erythrodermic, and psoriatic arthritis. Most people suffer from plaque psoriasis, which leads to the white, red, or gray scaly patches of excess skin that are most commonly associated with psoriasis. The large patches of excess skin typically appear on the elbows, knees, lower back, and scalp.
Guttate psoriasis is the second most common form of the disease. Sufferers with this condition typically notice small red spots. Most people develop this form of the disease as children, and it can be triggered by strep throat, stress, an injury, infection, or certain medication. The red spots are typically separated and appear on the torso and limbs. However, guttate psoriasis spots can also appear on the face and scalp. Guttate psoriasis spots are not as thick as plaque psoriasis patches, but without treatment, guttate psoriasis can develop into plaque psoriasis.
Inverse psoriasis, also known as flexural psoriasis, typically appears in the folds of the skin. This type of psoriasis appears red, smooth, and shiny. You may notice signs of inverse psoriasis in the armpits, under the breasts, and around the genitals. The sweat and moisture in these folds can stop the excess skin from shedding, making this form of psoriasis very uncomfortable. The majority of people who suffer from inverse psoriasis usually have another form of psoriasis impacting other parts of the body.
Erythrodermic psoriasis, sometimes called exfoliative psoriasis, is extremely rare. People suffering from this form of psoriasis often look like they have a severe burn. In many cases, this condition is treated on an emergency basis, and you may need to stay in the hospital during treatment. Erythrodermic psoriasis often covers large portions of the skin, can prevent the body from regulating temperature, and the skin often flakes away in large patches. This form of psoriasis typically develops as a result of untreated pustular psoriasis, widespread and poorly managed plaque psoriasis, severe sunburn, skin infections, severe stress, or the abrupt discontinuation of treatment for other forms of psoriasis.
Psoriatic arthritis affects about 1/3 of those people diagnosed with psoriasis. Because psoriasis suppresses immune function, it can attack the joints as well as the skin. In most cases, patients have side effects impacting the skin before they experience arthritic symptoms. Most people with psoriatic arthritis experience the worst symptoms in their hands.
Related: How to Manage Psoriasis in Cold Weather
Myth #5 Psoriasis Only has one Best Treatment
Depending on the type of psoriasis, you will receive a customized treatment plan to manage your symptoms and help you to look and feel your very best. Treatments utilized for the common forms of psoriasis include:
- Plaque psoriasis – treatment begins by identifying your triggers like stress or sleeplessness. You may also want to use cortisone cream or ointments to keep the skin moisturized. Vitamin D creams and topical retinoids can also be effective. As can medications like tazarotene or light therapy using UVA or UVB rays.
- Guttate psoriasis – may be caused by bacterial infections, so antibiotics are used to treat this condition in addition to topical ointments, light therapy, and/or oral medications.
- Inverse psoriasis – in addition to traditional therapies recommended for plaque psoriasis treatment, your dermatologist may also need to apply medication that reduces yeast or bacterial growth.
- Pustular psoriasis – depending on the size of the affected area, a dermatologist may recommend a number of different treatments. For smaller patches, over the counter or prescription corticosteroid creams are applied. For larger patches, oral medications or light therapies may be necessary. Treatments that address the causes of your pustular psoriasis may also be necessary.
- Erythrodermic psoriasis – treatment for erythrodermic psoriasis usually requires hospitalization to get the symptoms under control. Then, a dermatologist will create a plan to manage the effects of this condition moving forward.
- Psoriatic arthritis – over the counter pain relievers like NSAIDs and ibuprofen may be effective to keep your pain under control in the early stages. A physician may also prescribe pain relievers, anti-inflammatories, or topical medications to control symptoms. Medications called disease-modifying antirheumatic drugs may also be used to reduce inflammation at a cellular level.
Myth #6 Only Adults Have Psoriasis
While psoriasis is much more common for adults, it still impacts kids. Studies indicate that 20,000 children under the age of ten are diagnosed with this disease each year in the U.S. Children with one parent who suffers from psoriasis have a 10% chance of developing this condition, and if both parents have some form of psoriasis, children have a 50% chance of developing psoriasis. If you and/or your partner suffer from psoriasis, you should make sure your child receives screening for psoriasis at least once each year.
Myth #7 I can Prevent Psoriasis
You can reduce your risk for psoriasis by maintaining a healthy weight, avoiding excessive stress, consuming alcohol in moderation, and quitting smoking or tobacco usage. However, even if you take all the right steps to reduce your risk for psoriasis, you may not be able to prevent it, especially if one or both of your parents have some form of this condition.
Living a Healthy, Happy Life with Psoriasis
Psoriasis is a serious autoimmune disease that can affect anyone. It’s important for people to know the facts about this condition, so they can recognize the warning signs of psoriasis and seek treatment as necessary. Increased awareness can also reduce stigma surrounding this condition, so people suffering from psoriasis can begin to feel more confident and lead happier and healthier lives.
Looking to Visit a Dermatologist for Psoriasis Treatment?
A skilled physician or dermatologist can help you to assess the early symptoms and side effects related to psoriasis. If you have a family history of psoriasis or you have experienced warning signs of this disease in the past, contact U.S. Dermatology Partners to schedule an exam today. We have multiple locations throughout the country, so fill out our simple online form to get in touch with us. One of our local team members will reach out to you shortly to answer your questions or schedule an appointment for you to visit us soon.
Find a location near me
or