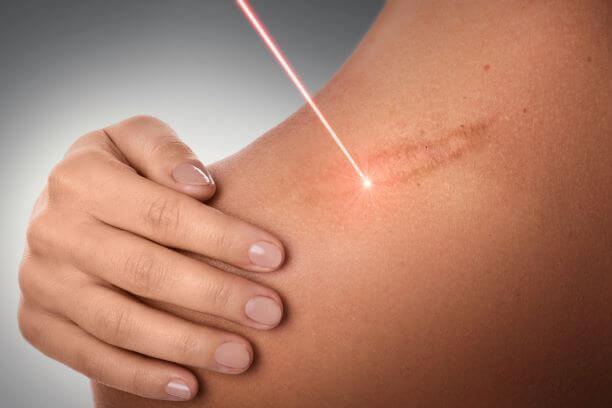
Some people relish their scars, proudly telling the stories of how they got them. However, many people want to eliminate their scars, especially scars that are in very noticeable locations. When scars really mar the appearance, impact movement, or cause other issues, there are options to reduce the visibility and correct other symptoms associated with problematic scarring. If you have one or more scars, you may want to have a dermatologist take a look, even if you don’t want treatment. There may be pain or other functional issues related to the scar tissue that we can help with.” In this blog, our providers have taken some time to discuss the answers to frequently asked questions about scarring, and we will be sharing them with you.
What are Scars?
Scars develop when the body needs to repair itself following an accident, injury, burn, or surgical treatment. Your skin is an organ, and like all the body’s other organs, it has a job. Skin creates a barrier between the body and external irritants and dangers. When that barrier is broken, the body goes to work repairing it as quickly as possible. The new skin cells are not always the same color or texture as surrounding skin, and we call this a scar.
Many people wonder why they only develop permanent scars after certain injuries. Scars develop when the deeper layers of skin cells are damaged. We tend to think of skin as one thing, but actually, you can think of it more like geographical rock layers. The top part, called the epidermis, is actually the oldest layer of your skin. These cells have developed from the inside, and over time, they are shed away making room for new cells from the deeper layers of skin. When damage occurs only to these top cells, there is not usually a scar. However, when skin damage goes deeper into the dermis layer of the skin where the new cells are still being formed, you’ll see these younger skin cells on the surface as your body rushes to repair itself. And, this is why scars will usually fade over time, as the damaged area begins to create new cells just like the rest of your body. But, unfortunately, scarring will not typically go away completely.
While many people also ask about different “types” of scars, scar types are really just descriptions of the scar’s appearance: color, shape, thickness, etc. that are helpful in diagnosis and treatment planning. The most common types of scars include:
- Erythema (redness)
- Hypopigmentation or hyperpigmentation (lighter or darker than normal skin color)
- Atrophy (sunken, divots into the skin)
- Hypertrophy (thickness)
- Keloid (protruding from the body)
- Contracture (contractile healing resulting in tightening and impaired function)
- Symptomatic (pain, itching, dysesthesias)
What is Scar Revision?
The term scar revision typically refers to the surgical treatment of scars. This process involves surgically removing the scar and then closing the wound in a different manner with the hope of improving the final appearance. However, there are many approaches to scar treatment (topical, laser, injections) that can improve the appearance of scars without surgical intervention. Treatments are tailored to address concerns associated with an individual scar, such as redness or thickness. If surgical scar revision is indicated, there are several different treatment options we may use, including:
- Skin grafts – removing skin for another part of the body to cover the scarred area.
- Skin flaps – a specialized type of skin graft that uses deep layers of tissue with their own blood supply to improve the appearance of the wound after it heals.
- Z-plasty – making a new incision in the skin to change the shape, direction, or position of the scar. This can relieve tension for contracture scars and reduce the visibility of scar tissue.
When Should a Patient Consider Scar Revision?
In most cases, scar revision is only recommended if there are serious functional or cosmetic concerns and other scar treatments will not be effective. Patients need to understand that the appearance of and symptoms associated with a scar can be improved with revision and other treatments, but the scar does not disappear completely. Individual response is variable based on numerous factors. Some of the reasons patients may want to consider scar revision include:
- Cosmetics – the appearance of scars, especially in very noticeable places like on the face, can be a factor that makes revision a good option.
- Function – scars, especially contracture scars, on the hands, near the eyes or mouth, or at other joints can impede function, making revision a necessary solution.
- Nerve damage – when scar tissue impacts the nervous system, the scar can have pain, itching, and other negative symptoms that make it necessary to perform revision to alleviate these side effects.
Does Insurance Cover Scar Revision?
Insurance coverage is often dependent on what procedure is being performed and what concern is being addressed. For example, laser treatment for redness within a scar is not typically covered by insurance. However, treatment of a thickened scar with intralesional injections often is covered. During a consultation visit with your dermatologist, you will get more details about the specific treatments available and whether or not your insurance covers them.
Is Revision the Only Option for Improving the Appearance of Scars?
There are many non-surgical treatment options for scars that may be recommended before surgical scar revision. These treatments are typically geared toward addressing a specific symptom of scarring. The following non-surgical options for treating individual side effects of scarring are recommended by our providers:
- For Redness – laser therapy
- For Hyper or Hypopigmentation – topical bleaching agents, other topical agents to improve skin tone, and laser therapy
- For Textural changes – laser therapy
- For Atrophy – injectable fillers, chemical peels, laser therapy, or radiofrequency microneedling treatments
- For Hypertrophy – laser therapy, injectable steroids, and other injectables (like 5FU)
- For Contractures – laser therapy
Is Scarring Preventable?
After a traumatic injury, cut, burn, or surgery, you are likely going to have some scarring, but if you talk to a dermatologist right away, they can offer you tips to help you reduce the risk for scarring and decrease the visibility of scar tissue. Some basic recommendations to minimize scarring include:
- Clean the wounds – wash and disinfect the wound at least once a day. When washing, avoid scrubbing or tugging at the skin, which can reopen the wound, increase the risk for infection, and cause greater chances of inflammation and scarring.
- Use petroleum jelly – applying petrolatum products like petroleum jelly creates a barrier over the wound. These moisturizing agents promote healing, keep the skin soft, and protect the wound from irritants.
- Cover the injury – keep the injury covered with a bandage to avoid further damage. When necessary, use hydrogel pads or silicone dressing to further protect the skin. You should also wear compression garments as instructed by your dermatologist. Change your bandages regularly, at least once a day, or anytime they feel saturated or look dirty.
Get Started with a Consultation at U.S. Dermatology Partners
There are U.S. Dermatology Partners locations in eight states, and you can request an appointment at any of our offices using our simple online form.
We are happy to be welcoming clients back to our practices, but if you’re still a little worried about health risks related to the coronavirus disease (COVID-19) pandemic or just like the flexibility of online visits, we also offer teledermatology. You can request your virtual visit using the online dermatology session request form.
However if you schedule your next appointment, the U.S. Dermatology Partners team can’t wait to see you!
Find a location near me
or