About Mohs Surgery
Overview of Mohs Micrographic Surgery
Originally developed in the 1930s, Mohs micrographic surgery has been refined into the most advanced, precise, and effective treatment for an increasing variety of skin cancer types. With the Mohs technique, physicians can precisely identify and remove an entire tumor while leaving the surrounding healthy tissue intact and unharmed.
Success Rate of Mohs Surgery
The Mohs procedure involves surgically removing skin cancer layer by layer and examining the tissue under a microscope until healthy, cancer-free tissue around the tumor is reached (called clear margins). Because the Mohs surgeon is specially trained as a cancer surgeon, pathologist, and reconstructive surgeon, Mohs surgery has the highest success rate of all treatments for skin cancer – up to 99%.
Advantages of Mohs Surgery
Mohs surgery is unique and so effective because of the way the removed tissue is microscopically examined, evaluating 100% of the surgical margins. The pathologic interpretation of the tissue margins is done on site by the Mohs surgeon, who is specially trained in the reading of these slides and is best able to correlate any microscopic findings with the surgical site on the patient. Advantages of Mohs surgery include:
- Ensuring complete cancer removal during surgery, virtually eliminating the chance of the cancer growing back
- Minimizing the amount of healthy tissue lost
- Maximizing the functional and cosmetic outcome resulting from surgery
- Repairing the site of the cancer the same day the cancer is removed, in most cases
- Curing skin cancer when other methods have failed
Other skin cancer treatment methods blindly estimate the amount of tissue to treat, which can result in the unnecessary removal of healthy skin tissue and tumor re-growth if any cancer is missed.
The Mohs Procedure
It’s helpful to know what to expect before you undergo any surgical procedure. Because the Mohs surgery procedure for skin cancer removal is somewhat complex, it can be reassuring to become familiar with the treatment process ahead of time.
Your Mohs Procedure
Surgeons usually perform Mohs skin cancer surgery as an outpatient procedure in the office, which has an on-site surgical suite and a laboratory for microscopic examination of tissue. Typically, surgery starts early in the morning and is completed the same day, depending on the extent of the tumor and the amount of reconstruction necessary.
You receive local anesthesia around the area of the tumor, so you are awake during the entire procedure. The use of local anesthesia versus general anesthesia provides numerous benefits, including preventing a lengthy recovery and possible side effects from general anesthesia. You are completely numb in the area of the surgery, though, so the procedure is comfortable.
After the area has been numbed, your Mohs surgeon removes the visible tumor, along with a thin layer of surrounding tissue. A technician then prepares this tissue and puts it on slides for your surgeon to examine under a microscope. If the surgeon sees evidence of cancer around the outer edges of the removed tissue, he or she takes another layer of tissue from the area where the cancer was detected. This ensures that only cancerous tissue is removed during the procedure, minimizing the loss of healthy tissue. Your surgeon repeats these steps until all samples are free of cancer. Although there are always exceptions to the rule, most tumors require 1 to 3 stages for complete removal.
After Your Surgery
When your surgery is complete, your Mohs surgeon assesses the wound and discusses your options for ideal functional and cosmetic reconstruction. Mohs surgeons understand that a good cosmetic result is an important part of the recovery process, and that’s why they work so hard to leave as little tissue damage as possible. If reconstruction is necessary, the Mohs surgeon usually repairs the area the same day as the tumor removal.
The Mohs Step-by-Step Process
The Mohs surgery procedure seems simple: the surgeon removes the cancer, carefully checks to be sure the he or she got it all, then repairs the wound. American College of Mohs Surgery members, however, train in and practice the complex nuances of this process for years so they are prepared to handle any situation they may encounter. This page describes the steps they follow for each Mohs surgical procedure.
Mohs skin cancer surgery is the most effective treatment for most types of skin cancer.
Step 1
The roots of a skin cancer may extend beyond the visible portion of the tumor. If these roots are not removed, the cancer will recur. A surgery starts with the surgeon examining the visible lesion and planning what tissue to remove. The patient then receives local anesthesia, and the Mohs surgery begins.
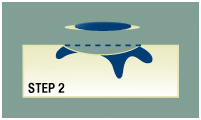
Step 2
The surgeon removes the visible portion of the tumor using careful surgical techniques.
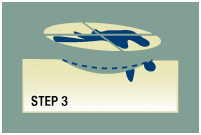
Step 3
The surgeon next removes a deeper layer of skin and divides it into sections. With the help of technicians, the surgeon then color-codes each of these sections with dyes and makes reference marks on the skin to show the source of the sections. A map of the surgical site is then drawn to track exactly where each small portion of tissue originated.
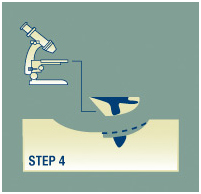
Step 4
In a laboratory, the surgeon uses a microscope to examine the undersurface and edges of each section of tissue in search of evidence of remaining cancer.
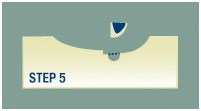
Step 5
If the surgeon finds cancer cells under the microscope, he or she marks their location on the “map” and returns to the patient to remove another deeper layer of skin — but only from precisely where the cancer cells originated. This method ensures that the Mohs surgery results in the smallest scar possible.
Step 6
The removal process stops when there is no longer any evidence of cancer in the surgical site. Because Mohs surgery removes only tissue containing cancer, it ensures that the maximum amount of healthy tissue is kept intact.
At this point, the surgeon discusses reconstruction options, should they be required, and then post-operative care. Mohs surgery recovery tends to be easily manageable because of the use of local anesthesia and the careful surgical techniques.
Why Does My Cancer Need Mohs Surgery?
Mohs surgery offers the highest cure rate among treatments for skin cancer. There are many other acceptable skin cancer treatment options including freezing (cryosurgery), scraping & burning, surgical removal (excision), and laser surgery, which all require the surgeon to estimate how extensively to treat the area around the tumor. There are many advantages to Mohs surgery compared to other skin cancer treatments including its high cure rate and cost-effectiveness. It is especially appropriate for skin cancers that:
- Develop on areas where preserving cosmetic appearance and function are important
- Have recurred after previous treatment or are likely to recur
- Are located in scar tissue
- Are large
- Have edges that are ill-defined
- Grow rapidly
Post-Operative Care
After a Mohs surgery procedure, most patients find the recovery process simple and easy thanks to the streamlined surgical approach that leaves surrounding tissue unharmed. Nonetheless, it’s common for patients to wonder what they can expect after a Mohs skin cancer surgery. It’s also important to use the post-operative period to plan an ongoing skin cancer detection strategy for the future.
Immediate Aftercare
After a Mohs surgical procedure, you may or may not undergo a repair process to mend the wound left by the surgery. A number of different reconstruction options exist, and instructions for aftercare are different depending on which approach the surgeon takes.
The surgeon and his or her medical team will provide you with detailed instructions to follow at home, and it’s important you do so in order to enhance your healing and final outcome. These instructions will include:
- Information about when to change bandages and how to clean the surgical site
- Medication information about prescription or over-the-counter pills or topical ointments
- A timeline for when you can return to certain activities, such as wearing makeup or exercising
- A schedule of follow-up appointments to remove any stitches and monitor your healing
- Recommendations for treating your Mohs surgery scar to ensure it heals and fades quickly
Because Mohs surgery is performed in an outpatient setting using only local anesthesia, immediate recovery generally involves little more than resting and simple wound care. Some patients may experience mild discomfort, bleeding, redness, or inflammation, but these are typically temporary and easily manageable.
Long-Term Care
Although Mohs micrographic surgery has an extremely high success rate that frequently prevents skin cancer from recurring at the same site, monitoring is still very important for Mohs patients. Once you discover that you are prone to skin cancer, diligence is crucial for detecting any new lesions that may form elsewhere on your body.
Mohs Surgery FAQ
Mohs surgery is the most effective treatment for most types of skin cancer. We have provided answers to several common questions about Mohs skin cancer surgery below.
Why is it called Mohs surgery? Is Mohs an acronym?
The term “Mohs” refers to Dr. Frederic Mohs, Professor of Surgery at the University of Wisconsin, who developed this surgical technique in the 1930s. The technique has undergone many refinements and has come to be known as “Mohs micrographic surgery” or simply “Mohs surgery” in honor of Dr. Mohs.
What is Mohs surgery?
Dr. Mohs recognized that a skin cancer often resembles the “tip of the iceberg” with more tumor cells growing downward and outward into the skin like the roots of a tree. These “roots” are not visible with the naked eye, but can be seen under a microscope.
Mohs surgery is a highly specialized and precise treatment for skin cancer in which the cancer is removed in stages, one tissue layer at a time. It is an outpatient procedure, performed under local anesthesia, and is distinguished by a specific technique of tissue examination that is unique to Mohs surgery. Although other surgical specialists may check excision margins, this form of pathologic examination of the tissue is not the same as Mohs surgery.
Once a tissue layer is removed, its edges are marked with colored dyes, and a map of the specimen is created. The tissue is then processed onto microscope slides by a Mohs histotechnician. These slides are carefully examined under the microscope by the Mohs surgeon so that any microscopic roots of the cancer can be precisely identified and mapped. If cancer cells are seen, an additional tissue layer is removed only in areas where the cancer is still present, leaving normal skin intact. This saves as much normal, healthy skin as possible.
Once the cancer has been removed, the Mohs surgeon will explain options for repair of the wound, including natural healing (granulation), stitching the wound together using a side-to-side closure, or using a skin flap or graft.
It’s important to choose a fellowship trained Mohs surgeon who is a member of the American College of Mohs Surgery. Mohs College surgeons have undergone at least 1 year of fellowship training beyond dermatology residency, which allows for additional experience in all of these specialized processes and techniques.
I don’t see anything after my biopsy. Do I really need to be treated?
Yes. Following a biopsy, your skin cancer may no longer be visible. However, the surface lesion that was removed can represent the “tip of the iceberg.” More tumor cells may remain in the skin. These can continue to grow downward and outward, like roots of a tree. These “roots” are not visible with the naked eye. If they are not removed, the tumor will likely reappear and require more extensive surgery.
Tumors that are neglected can spread deeply into the skin and invade nearby structures. On rare occasions, these cancerous cells can metastasize to lymph nodes and other organs in the body.
Why does my skin cancer need to have Mohs surgery?
Mohs surgery has the highest cure rate. It is appropriate for most skin cancers and especially suitable for skin cancer that:
- Is in an area where it is important to preserve healthy tissue for maximum functional and cosmetic result
- Was treated previously and has come back
- Is located near scar tissue
- Is large
- Does not have clearly defined edges
- Is growing rapidly or uncontrollably
- Is of an aggressive subtype (i.e., sclerosing or infiltrating basal cell carcinoma)
- Develops in organ transplant or lymphoma patients
Please note: the above list is not exhaustive of all of the instances where Mohs surgery is the most appropriate option for your skin cancer.
How long does Mohs surgery take?
Although Mohs surgery can take longer than other techniques to perform, advances in technology, such as automated staining of tissue samples, have made it quicker. While it is impossible to predict exactly what timeframe to expect for each Mohs surgery procedure, the entire procedure usually lasts several hours. Rarely, clearing the tumor and reconstructing the defect can take the better part of a day. A consultation with the Mohs surgeon prior to your procedure will allow for the surgeon to understand the unique qualities of your situation and enable him/her to more clearly estimate the extent of the timeframe for the surgery.
Will Mohs surgery leave a scar?
Yes. As will any treatment for skin cancer, Mohs surgery will leave a scar.
Mohs surgery preserves as much healthy skin as possible and maximizes options for repairing the surgical defect, once the tumor is completely removed. Once the Mohs surgeon has completely removed your skin cancer through Mohs surgery, reconstruction for optimizing the final functional and cosmetic result becomes the highest priority. Generally, a post-surgical scar improves with time and can take up to 1 year or more to fully mature. As your surgical site heals, new blood vessels can appear and support the healing changes occurring underneath the skin. This can result in the reddish appearance of the scar. This change is temporary and will improve with time.
In addition, the normal healing process involves a period of skin contraction, which often peaks 4 to 6 weeks after the surgery. This may appear as a bumpiness or hardening of the scar. On the face, this change is nearly always temporary and the scar will soften and improve with time. If you have a history of abnormal scarring, such as hypertrophic scars or keloids, or if there are problems with the healing of your scar, injections or other treatments may be used to optimize the cosmetic result. Your Mohs surgeon is available for you throughout the healing process to discuss any concerns that may arise.
Mohs College FAQs
The American College of Mohs Surgery (ACMS), founded by Dr. Frederic Mohs, has established the highest standards of training and patient care for Mohs surgery.
My surgeon is a member of the American Society of Mohs Surgery (ASMS). Is that the same as the ACMS (Mohs College)?
No. Only ACMS physicians are required to undertake an additional 1 to 2 years of rigorous fellowship training that the American College of Mohs Surgery requires of its surgeons to become members.
Why is it called the “college” of Mohs surgery?
Professional medical associations use many different terms to describe their organization. Some examples are the American Medical Association, the American Academy of Dermatology, the American College of Mohs Surgery, and the American Society for Dermatologic Surgery. All are medical professional associations, but each has its own set of member eligibility requirements.
In the case of the American College of Mohs Surgery, to be admitted, a member must have completed an approved fellowship in which they have participated in the surgery of at least 500 patients under the supervision of an approved Mohs surgery instructor.
So the Mohs College (ACMS) isn’t an actual school with a campus?
Correct. The American College of Mohs Surgery is a membership organization of 1,400 surgeons who perform Mohs surgery and are committed to advancing the education, research, development, and application of standards and guidelines to advance this specialized procedure.
What is a fellowship trained Mohs surgeon?
The ACMS fellowship is an additional course of study for 1 to 2 years that provides the opportunity for surgeons to develop good judgment and become highly skilled in Mohs surgery. This includes the following:
- Excising skin cancers and creating precisely-oriented microscopic maps
- Interpreting slides containing tissue removed during the procedure
- Repairing the surgical defect, which involves exposure to and development of a wide repertoire of reconstructive techniques.
During the fellowship, each surgeon-in-training must participate in a minimum of 500 cases under the supervision of a Mohs College approved, fellowship-trained instructor (surgeon).
What are the membership requirements for the ACMS?
An MD or DO must have completed a 1 or 2-year Mohs fellowship at one of the 70+ Mohs training programs across the country. Most are 1-year programs, but the programs are identical in all but the length of time it takes to complete them. All Mohs fellows must complete at least 500 Mohs surgery cases during their fellowship. Fellows-in-training must perform most of these cases under the guidance of the training program director, but in a minimum of 125 cases, fellows must be the “primary” surgeon.
How long has the ACMS been around?
American College of Mohs Surgery was founded in 1967 as the American College of Chemosurgery by Dr. Frederic Mohs, who pioneered the technique. Through the ensuing years, the Mohs micrographic surgical process was refined, and in 1988 the membership changed the name to the American College of Mohs Micrographic Surgery and Cutaneous Oncology, noting the full spectrum of their work. The membership voted on the 40th anniversary of the College in 2007 to shorten the name to make it more user-friendly to the general public.